Forum Replies Created
Al n Casy,
I am sorry to read this. This has been very sudden and difficult for you. You must be very worried.
Some of this is complicated to understand, like your Malti’s genetics, but some of this is quite easy to understand.
Each of us, whether we are dogs or humans, inherits certain characteristics that determine our resistance to stress and our ability to remain healthy.
In the dog world, there are an increasing number of diseases and conditions that dogs (and especially certain breeds) are expressing. Allergies and orthopedic conditions are two that you might understand. Autoimmune diseases is another of these conditions. AIHA, IMHA and bone marrow failure are autoimmune conditions that can be expressed when the immune system that has been challenged by something in the environment that it finds toxic.
In your case your Malti was exposed to multiple flea, tick and parasite medications in a very short time. This was overwhelming to her very delicate immune system. Seeing that she had at one time in her life been very sick, it is quite possible she was still in a very sensitive state. She has responded to this stress with an autoimmune condition that is leading the immune system to mistakenly attack “self” and in this case it is destroying red blood cells.
I know you are reading a lot of things right now on the internet and it is very easy to become overwhelmed. While you need to know some details to make decisions for your Malti, you also don’t have all the time in the world to learn everything about this.
Multiple sources can have conflicting information and that will be very confusing. Your vet has not explained this very well to you either and probably would be defensive if you suggested that he shouldn’t have administered these flea, tick and parasite medications.
We developed this site with two goals in mind, to help anyone, everyone who has a very sick dog. We have all been through this with our own dogs and we have experienced the same terror and confusion that you are having. Secondly, we have spend years researching and learning about these conditions so we can help owners make decisions that will help their dog live. The information we provide to you is sound and accurate. When we aren’t sure we say that as well. We have consultants that we can check our accuracy with.
First, put the cancer business out of your mind for now. It is more likely right now, that this is exactly what it often is, an autoimmune response to the stress of a recent application of flea, tick and parasite medication. It’s not quite as simple as that, but that was the tipping point that led to this.
We don’t necessarily want to tell owners that they should not trust their vet, but in some cases, if an owner just doesn’t get a good feeling we do suggest finding another vet, or perhaps consulting a specialist. I feel your anxiety and I think there was a little bit of half truths in your vet’s behavior that has led you to feel unsure of what he is saying and doing.
There are two things you could do right now. Find a specialist and get a second opinion. We also suggest that in lieu of this expense that you do a consultation with Dr. Dodds and we have a link to that page here on the website. Her fee is inexpensive and she can be quite helpful by email with you. We have all received life saving help from Dr. Dodds. Chance, who the website is in memory of, was saved by Dr. Dodds. Think of this as a second opinion, just as you would get for a member of your family, and your vet should welcome that opinion.
Go to this link
https://www.secondchanceaihadogs.com/hemopetresources/
And select the picture of the Owner Consultation Form. This will take you to the website where you can request a second opinion from Dr. Dodds.
At the bottom of this page you can also read about Dr. Dodds and how she has helped dogs for many years.
The meds are ok for now, but there may be some adjustments that could be made. I would like you now to ask your vet to approve the use of some kind of stomach acid protection. You can also use any over the counter generic such as pepcid. For this little body, one tablet a half hour before the first meal of the day with prednisone in it will work. Make sure the Atopica is given away from meals, with no food, by at least 2 hours on either side.
Your Malti is going to have side effects from the prednisone, notably more drinking, eating and peeing. Do not get upset if she makes a mistake in the house. Take her out more frequently and sleep with her if you have to so that she can get out quickly. She is going to feel very uncomfortable.
There are other suggestions about diet and other supplements but right now just use some very simple foods like plain cooked chicken and overcooked rice. A little yogurt and perhaps an egg.
Meanwhile, read some of the information on the website. You can browse the Second Chance Resources, AIHA Terms, watch two short introductory videos and read Our Stories.
Do I think she will survive? Yes, I have seen many dogs that have caring owners survive. Because you are a good mommy, you noticed something was wrong and you took immediate action. That has saved her life.
Now to help her suppress this crazy immune system you need to use some harsh drugs that have some lousy side effects. But this will save her life also. We need to keep her healthy while she is being treated. That means easy to digest simple food, lots of clean water, low stress at home. All good nursing care. Please begin to keep a diary in the kitchen and note all times when you are giving meds, the dosages and the names. Mark down things like potty times, symptoms you notice etc. We will need to add a few supplements to correct for some of the side effects on the body from the prednisone.
Vally will help you create a medication chart so you can sort this all out. Do not fret, we know what must be done and we will guide you.
What questions do you have?
my best patrice
Sara,
Actually, dogs with a predisposition to autoimmune atophy tend to express this early in their lives, around 2 or so. Chance did this. It was a sign that something else loomed in the future, his autoimmune bone marrow failure.
Chance’s allergies came on with a vengeance and we were just completely flummoxed. We did not have a clue in 2000 why this could be happening to a young puppy. We certainly wasted a lot of time dancing around the issue, a bit in denial. I tried so many over-the-counter things, but none of them worked. The vet suggested we see a veterinary dermatologist and we were very hesitant about that. It would be an expensive visit.
Finally, when our lives became upside down because of his allergies, we did relent and see the vet dermatologist specialist. There were two sets of tests, a blood test and a scratch test. The blood test is imperfect and she warned us it would not be very specific nor improve treatment. The scratch test was very specific and it showed a whole panel of things he was allergic to. From this, they eventually developed his own personal serum that became his allergy shots.
She also wanted us to do a elimination diet, but I was savvy enough, like you, to realize that he was only bothered during the spring and the fall, and much less the rest of the year. I did remove chicken from his diet because he had always refused to eat it anyway and I think he was allergic to it. I had fed him a raw diet, per the breeder, right from the start. For the bulk of his life after this he got raw meaty lamb bones or pork shoulders, no chicken.
So the dermatologist told us that the best treatment would be allergy shots. (This was long before Atopica came to market.) Boy were we reluctant about that! In the end, I knew I had to do it for him, his life was miserable. So this was wildly expensive and the schedule and dosing was very complicated and specific. She also told us it would take a year, possibly longer, for the shots to become effective. Until then we had to use other measures to control his symptoms.
She gave me a long list of approved antihistamines with their canine doses and insisted we use Malaseb shampoo. She also prescribed Temaril-P (Trimeprazine 5mg, Prednisolone 2mg) for us to use during the worst times. So for maybe 2-3 weeks in the spring and fall I would dose him with this to allow his skin to heal and to give him relief from the agony. This medication was a life saver. I still highly recommend it to owners whose dog’s allergies return after being in treatment for AIHA but have discontinued the prednisone, since the dose of prednisone is quite small.
He began to respond to the allergy shots the following year and from then on, he was virtually free of allergic symptoms other than a little eye gooping during the worst pollen season. We also continued the malaseb shampoo throughout his life which really improved his skin and coat. This shampoo fights bacteria but it also fights yeast. Dogs that work themselves raw significantly increase the growth of yeast on the skin and this burns terribly, making it a vicious cycle of destruction. So part of treatment had to include stopping the dog from licking and also treating the yeast with Malaseb about every 10 days which works great.
All this manipulation of his immune system was not a good idea, but that wasn’t understood as well back then. This specialist told me that dogs with serious allergies were sometimes even put down because their lives were so miserable. Seriously. So for us, shots were a choice we made for his comfort, not for his longevity.
Atopica came on the market around 2007. This was the year that he developed autoimmune bone marrow failure. A specialist was clueless about how to treat him and only prescribed prednisone. Over several months his health diminished on very high doses of prednisone. It was only when we contacted Dr. Dodds did she insist he be put on cyclosporine. I struggled trying to find any of this human medication locally. It wasn’t available. My vets were working with Dr. Dodds and offered “we have Atopica on the shelf, will that work?” She replied that this was a perfect solution. So this was probably the first time a dog being treated by Dr. Dodds used Atopica, packaged for canine atophy! The capsules were so easy to dose and I could get them right at the vets’ office.
You are correct, cyclosporine (Atopica) is prescribed now for dogs with atopic allergies, it was researched and tested for marketing for canine atophy, not for autoimmune diseases, but is now used, off label, for many different conditions other than allergies! It has saved many dog’s lives that would have been put down in 2000 for intractable allergies. Dosing is important with this drug. There is a ramp up period where the drug is dosed at a higher dose to “load” the system and then the vet will experiment with a lower maintenance dose to see what works well for the specific dog. The idea is to control the atophy at the lowest maintenance dose possible.
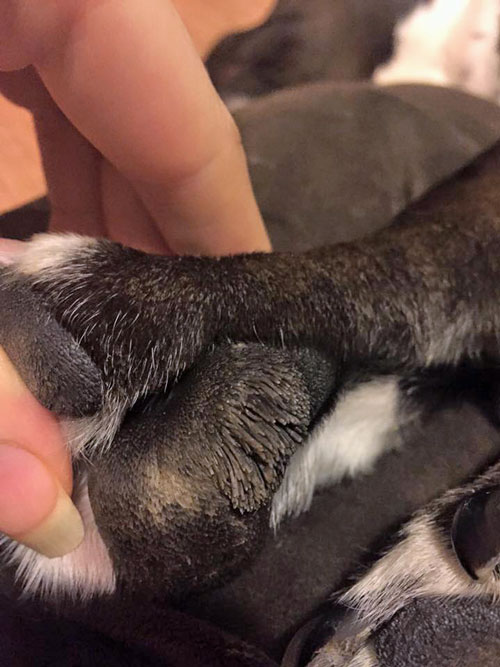
I also noticed with Chance taking high dose Atopica that he did develop what are called hyperplastic skin lesions. They looked pretty horrible but he never itched his skin or had any irritation from these growths. Many dogs do get these and similar skin conditions.
The action by which cyclosporine works (a fungus) is to disrupt the growth of rapidly growing cells, in this case the T-cell lymphocytes that are responsible for autoimmune attacks like allergies or AIHA. This disruption of fast growing cells is also directed at skin cells (epithelial) and thus you can see this abnormal growth not only on the skin but also on the gums and sometimes the pads of the paws. The skin’s genetic blueprint for making cells becomes altered and “skin” looks very different than what was planned.
“Hyperplastic skin lesions occasionally develop during treatment with cyclosporine A. Most of the lesions resemble those of psoriasiform lichenoid dermatosis, although papillomavirus can be detected in some instances.”
But here’s some specific and important information I found about Springer Spaniels and a hereditary condition Psoriasiform-lichenoid dermatosis.
“Psoriasiform-lichenoid dermatosis is a rare skin disease of Springer Spaniels characterized by symmetrical papules, plaques and nodules.
(see picture here: )
http://www.vetbook.org/wiki/dog/images/a/ab/Psoriasiform01.jpg
The marked breed predilection suggests heritability. The aetiology is not known but this disease may represent an atypical Staphylococcus pseudintermedius infection.
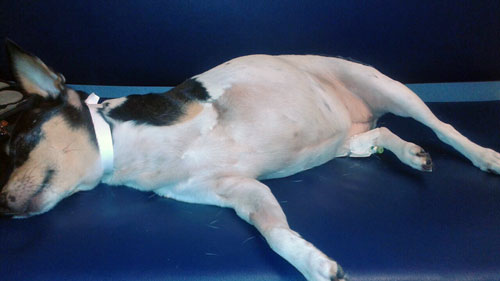
The condition is primarily observed in young dogs with lesions on the pinnae, ventral truncal region and genitals.
Over time, the lesions progress to hyperkeratotic lesions with adherent crust and keratinaceous debris. Follicular casts may be observed.
Chronic cases resemble severe seborrhea with malodor a definite part of the history and Staphylococcal pyoderma may be seen as a secondary factor.
Resolution may be achieved with prolonged courses of cephalexins such as Cefovecin. The use of cyclosporin, which is used for lichenoid keratoses in other breeds is usually unrewarding.”
So this resembles what you are describing and matches your breed. I think this is worthy of mentioning to your vet and perhaps a visit with a dermatologist specialist is called for. I think attempting to treat a condition like this with acupuncture is an unfortunate redirection away from medicine and proper clinical diagnosis.
Since this condition is considered relatively benign , and if they are causing no discomfort, then antibiotic treatment is optional. That is your choice after discussing it with your vet. There could still be some degree of atophy. The shampoos used about every 10 days may be enough to keep the itching under control.
my best
patrice
Sara,
It is extremely common for conditions like allergies to be suppressed while on prednisone. Other conditions, for instance arthritis, are also improved while on prednisone. This is due to the antiinflammatory behavior of prednisone.
So excited owners can’t wait to get their dog’s prednisone reduced only to find that the dog seems to be feeling worse, arthritis pain returns or allergic symptoms return.
So what seems puzzling to you, this happening once the pred is removed is actually to be expected.
However, staph is something that usually increases as the body’s immune system is suppressed.
I don’t like the sound of the way it looks. Some types of staph can become more serious than others. One particular strain is called MRSA. I mention that in the link that Vally sent you. MRSA can be very difficult to treat in both humans and dogs.
I think right now it would be wise to see a dermatologist just to be sure that you are providing a treatment that will clear this up effectively.
Chance had life altering allergies and it was very difficult for us to treat him. I know how heartbreaking it is to see a dog scratch and chew themselves down to raw skin.
I would suggest using a medicated shampoo like chlorhexidine dog shampoo. I have used Douxo Chlorhexidine PS Shampoo with great success, also Malaseb was critical in easing the itch and healing the skin. Check with your vet first about this, but I think they will agree that this will calm the skin down.
my best
patrice
Sheena,
I am so sad to read this.
There is no one else that I can think of who could have taken Ollie in and given him such a wonderful life. Without you, he would have been a lost soul always looking for his perfect friend.
His life was complete, surrounded by the family he loved, and his pal Worzel to hang around with. This is an empty space that nothing can fill.
I hope that he is always with you each day, a sparkle of light through the window and a light tap at the door.
Please accept my deepest condolences.
patrice
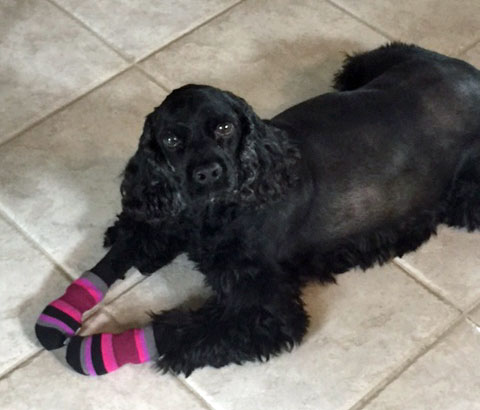
Ollie’s Beautiful Eyes

Ollie’s Best Friend Worzel

Ollie
We have a secret, you and I, that no one else shall know,
for who but I can see you lie each night in fire glow?
And who but I can reach my hand before we go to bed,
and feel the living warmth of you and touch your silken head?
And only I walk woodland paths and see ahead of me,
your small form racing with the wind so young and free.
And only I can see you swim in every brook I pass
and when I call, no one but I can see the bending grass.
Lauren,
I know that it’s critical because it was an integral part of Chance’s treatment.
You can find a great deal of information about hypothyroidism on this page.
https://www.secondchanceaihadogs.com/canine-hypothyroidism-resources/
Jean’s reference page that she sent me is a document on this page. Look for the graphical representation of a thyroid molecule. You can open this document in a separate tab and print or save from there.
Dogs with non regenerative anemia do not have rapid declines in PCV HCT, their losses are slow, over time. This is not non regenerative anemia.
I don’t know all that has been checked but I would suggest also looking for internal bleeding. Ruptured spleen or spleen accessory growth, gastrointestinal bleeding, tape worms, ulcers. In these rapid blood losses there is a delayed regenerative response, that is expected.
My best Patrice
Lauren,
With ANY level of anemia (that would be a PCV or HCT below 38% and less than 5.5 million red blood cells), in order to be considered regenerative the absolute number of reticulocytes must be equal to or greater than 60,000 or 1%. And indeed, when there is no anemia (PCV HCT equal to or greater than 38%) the average normal value of reticulocytes stays steady at about 1%, 60,000 absolute. This applies to humans as well as canines! And the body carefully modulates this values with intricate feedback loops. It is an amazing process.
The greater the anemia, the higher this value must be to be considered adequate regeneration. This is the hardest part to understand. There are several math formulas that help determine the proper level of regeneration that must occur depending on the seriousness of anemia.
For example a dog has a PCV HCT of 18%, which is considered severe anemia. Ideally it would be nice to see values of absolute reticulocytes upwards of 300,000-500,000 and percentages like 3-4-5%!
With bone marrow failure, Chance had, the first time we were at the vets, a PCV of 30 and he had only 13,000 reticulocytes. This set off a trigger of a very dangerous indication that something was very wrong. And he also had extremely low white blood cells so he was also considered to have neutropenia, failure to make white blood cells. Luckily he was making platelets or it would have been very severe, this would be called pancytopenia, the loss of all blood cell lines. You can read Chance’s story, along with all the other stories here:
https://www.secondchanceaihadogs.com/our-stories/chance/
Reticulocytes are immature red blood cells, larger than normal because they contain the RNA from their development stage. When the red blood cells are stained with purple and viewed under a microscope they have a reticular appearance (spotty) and that is why they are called reticulocytes!
It takes reticulocytes about 3-5 days to mature, drop the RNA and become ready to begin carrying oxygen in the hemoglobin molecule to the body cells. So if you look at a CBC and see a large value for reticulocytes you can expect within a week to see a huge increase in the number of red blood cells and a decrease in the reticulocyte values, does this make sense to you?
It is unfortunately more common now-a-days to see canine bone marrow failure due to an autoimmune attack at the deepest level of the bone marrow, the precursor cells. This was Dr. Dodds determination with Chance.
I am not, nor is she, a proponent of immediate bone marrow biopsies when a dog is non-regenerative. We prefer to recommend a trial of the bone marrow failure protocol to see if there is any response to a higher dose of several immunosuppressives (including cyclosporine). If there is a response, then it confirms the diagnosis of an autoimmune attack on the bone marrow. If there isn’t a response then further testing can possibly include a bone marrow biopsy, among other tests. It is preferable in the beginning to save your money for one or more blood transfusions.
We put Chance on Dr. Dodds’ bone marrow protocol and within 3-4 weeks he began to respond with moderate regeneration. It took months after that for him to recover completely from his condition and the side effects of the drugs.
Please upload your CBC on the Urgent Advice page. I will look at it, do some math and let you know what I find.
If you have any questions about what I have written, please let me know.
my best, patrice
The PTT is Partial thromboplastin time (PTT.) It is a blood test that looks at how long it takes for blood to clot. It is used primarily to investigate unexplained bleeding or clotting.
The high results can mean:
1. Deficiency of blood clotting factors
2. von Willebrand’s disease (a disorder that causes abnormal blood clotting)
3. DIC Disseminated intravascular coagulation (a disease in which the proteins responsible for blood clotting are abnormally active)
my best, patrice