Forum Replies Created
Taylor,
Yes, I was expecting to actually hear this from you at some point. No, they don’t know what they are looking at and are confused. I do know what is probably going on and I need to see the lab results before I confirm this.
Don’t let them upset you. For sure I was horribly upset in the beginning and it certainly made for a lot of stress in our lives. There is a very complex but scientific explanation for what may be happening. When we have more time you and I can discuss this at length.
The most important thing for you to worry about right now is getting him stabilized and eating properly again. But right now, the diet needs to be appropriate for his struggling kidneys.
A good friend Mary Straus has a great website, Dogaware, and she covers kidney conditions and diet very well. You are going to be overwhelmed if you try to read this whole page and understand it all, just browse through and get a good idea of how the kidneys can be compromised.
http://dogaware.com/health/kidney.html
This advice on her page is very important:
“Let me start by telling you what not to do: do not put your dog on a prescription kidney diet.
A reduced phosphorus diet is not needed or beneficial until creatinine rises above 2.0 mg/dL (180 umol/L) or fasted blood phosphorus level rises above 4.5 mg/dL (1.5 mmol/L).
So we need to see your chem screen reports asap to know what the creatinine levels are.
Here is her information about diet and dogs with kidney disease. Keep in mind this may be a temporary situation, not kidney disease!
http://dogaware.com/health/kidneydiet.html
And here is Mary’s suggestions for diets for early to moderate kidney disease, understanding this may not be kidney disease but that the kidneys need to have a light load right now.
http://dogaware.com/health/kidneysamplediet.html
Right now I would use her sample diet but do not use red meats or beef liver, which could put a load on his liver, I would use eggs and egg whites plus some steamed white fish. But stick with the same basic concepts she covers. Y
You don’t need to get super concerned about grinding egg shells, crumble them with your hands or put them in a plastic bag and roll them with a pastry dough roller. For grains I recommend getting plain old sushi rice at the grocery store and let it cook in plenty of water until it is quite mushy, use the liquid in the meal also. Butter can be a vehicle to get pills down. Yogurt should be plain and that makes a great treat.
The ultimate goal is to reduce phosphorous in the diet, do you understand this part that she explains in the introduction?
Whatever help you need, let me know,
my best patrice
Taylor,
These growths are fragile and can bleed and heal many times, causing a continued troublesome anemia. Rupture in these cases is a strong possibility and it’s great they caught it before that happened.
Chance, whom I named this site after, had exactly the same thing, a large benign growth on his spleen. I have gathered a great deal of information about these conditions since 2007. You can read his story under Our Stories.
Because of this information I suspect we may find a slightly different situation for Harley than the usual IMHA. Once I see the test results I will know more.
my best, patrice
Hi Taylor,
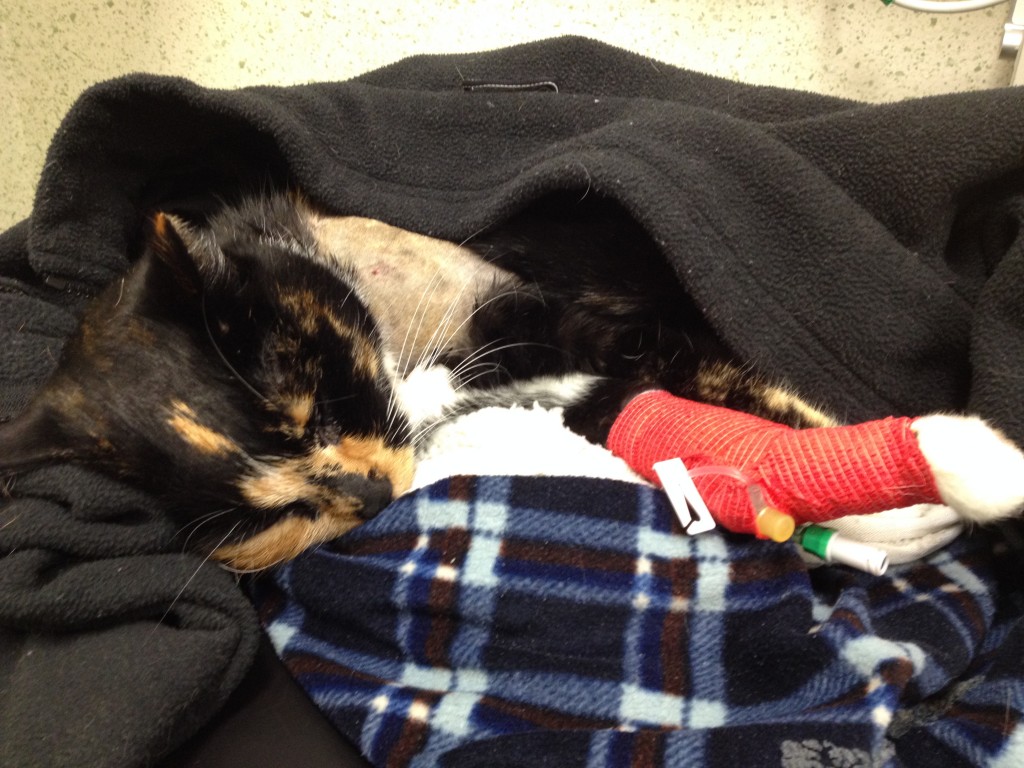
I am sorry to read about Harley. You must be so worried and confused.
I’d like to know a little more about this growth on the spleen. You say he was suddenly ill and then they removed the spleen and the growth in an emergency surgery, am I correct?
There can be different growths on a spleen. Benign growths are not uncommon. Malignant growths can also be found on the spleen. The main reason for this is that the spleen is a blood filled organ and that is a nice environment for cells that want to have plenty of nutrition to grow quickly. Unfortunately rapidly growing cells on the spleen tend to be unstable as they get larger. This means that they can be more apt to rupture and bleed. Approximately 60% of splenic growths are benign while the rest are likely to be hemangiosarcomas, a malignant tumor growth common in older dogs.
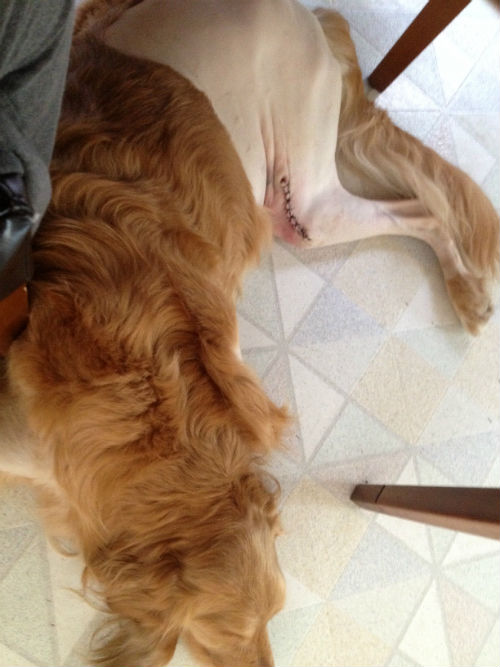
It sounds like Harley’s growth ruptured suddenly, making him quite ill. They most likely removed the spleen and the growth so that he would not lose so much blood. It sounds like they appropriately sent out the growth for a cytology to determine if the growth was benign or malignant and the report was that it was benign, am I correct?
In the case of a benign growth that has ruptured, removal of it and the spleen would be an appropriate treatment. A dog can survive quite well without a spleen, though from that point on they are less able to fight off a certain tick disease called babesiosis. However in some cases, which are more complex, the removal of the spleen and the growth can lead to conditions similar to but not quite like IMHA. I would like to see several lab reports, CBC and chem screens, that were done prior to the surgery and also post surgical to be able to see what exactly is happening here.
Surgery is quite a shock to the body and this was a tough surgery on a little body. It is quite understandable that he is not feeling well at all. Prednisone is a potent drug and the side effects are very pronounced. It is quite normal for vets to use this drug as an emergency treatment for many conditions.
So the question I have is this truly a confirmed case of IMHA? Did they remove the spleen because they felt the spleen was contributing to the IMHA and then discovered the growth? Or did they remove the spleen because of the benign growth and the IMHA developed afterwards?
The kidneys are very sensitive to the load they receive when there is a destruction of many red blood cells in the body. The destroyed RBC cells release a great deal of hemoglobin, the contents of which must be processed as wastes by the liver and kidneys. This load can overwhelm the kidneys. Putting Harley on IV fluids can help flush the system. This most likely is a temporary situation.
Many dogs with anemia do express a temporary heart murmur as the heart attempts to work harder to pump more poorly oxygenated blood to the body cells. Anemia, by definition, is less oxygen being carried to the body cells. In this case it is due to a smaller number of RBC.
So the treatment needs to address the reasons for why there are less red blood cells. Transfusions can help stabilize a dog that has severe anemia. I am positive that they have already given at least one transfusion during the surgery. Subsequent transfusions will be helpful provided that the vet types and matches the transfused blood properly.
Yes, the goal is to stabilize Harley right now. The body is very resilient and dogs can be quite amazing in their ability to recover their homeostasis. When he is released to home we can help you provide some great home nursing care to him.
Help me by uploading the test results on the Urgent Advice page. Please limit the attachments to 3. We can use email to gather the rest.
What questions do you have for me?
my best, patrice
Ann,
I’m sorry to read about Minnie. It sounds like she has stabilized and that is a good sign.
This is a serious condition and the drugs that are needed to control this have some side effects that are not pleasant. It is completely understandable that she is not very social right now. If there is one thing for sure, dogs that feel very ill will behave in a way that you have never seen before. Every dog that has been treated for these hematological conditions behaves similarly. And each dog has a different tolerance for the anemia and for the drugs. So one dog may be able to tolerate a PCV of 12 quite well, while another dog will be so ill they can hardly stand.
If you look above at the menu items you will see Our Stories, this is a selection of many owner’s stories about their sick dogs. You will see Chance’s Story, who this site is in memory of. Chance, a Giant Schnauzer, had terrible allergies starting at the age of 2. It was a life altering experience for our household. At that time the only effective treatment was to see a veterinary dermatologist and test for allergies with skin and blood tests, just as we do with humans. They developed a special serum for him and I gave him allergy shots for many years. It helped quite a bit and we thought he was doing well.
However, when he was about 7 he seemed to slow down, he was sluggish and gained weight. I was not sure what was happening to him and eventually we discovered that he had a large growth on his spleen. This (7 lb)benign growth and the spleen was removed and the vet felt this was curative. However, within a month, his blood tests showed he was not making red blood cells or white blood cells. It was indeed a very ominous diagnosis. This is actually one of the forms of canine autoimmune hematological disease, similar but different to AIHA IMHA.
Chance was on prednisone, the same as Minnie, but he did not respond well. It was several months of treatment and he became more anemic. I was in contact with Dr. Dodds and she sent me her protocol. Once we started him on cyclosporine he improved and eventually recovered even from the side effects of prednisone. Chance lived another good three years to the age of 12 and passed from an unrelated heart condition. Chance was not the same dog coming out of this that went in, as is the case with nearly every dog who is treated, but his will to live and his enjoyment of life was not reduced one bit. We gave him a good life and he wanted for nothing.
What I do know now, after studying these canine hematological diseases for a very long time, is that dogs are genetically prone to expressing these diseases if they are of certain breeds and or they are prone to autoimmune diseases. This includes allergies and many other autoimmune condition that affect dogs. Chance was set up from an early age because of his allergies to go on to express a far more serious autoimmune disease later in life.
Why? Because dogs have an accelerated metabolism and thus they live shorter lives. They develop the kinds of age related conditions that humans might at a much younger age. If they have a genetic makeup that is more fragile the environment will most certainly challenge their immune system. And by environment, I include all aspects of a dog’s life, from diet to veterinary care (flea, heartworm and tick prevention included) to where they walk, parasites, viruses, bacteria and other diseases they may be exposed to. Dogs with allergies to their environment are at high risk when exposed to pollen and molds etc.
Minnie is 6 and a Dachshund. This breed has a genetic disposition to canine atopic allergies and autoimmune diseases, among other conditions. In addition AIHA IMHA are more prevalent in middle-aged spayed female dogs. The risk of acquiring the disease is more common in May and June, this is widely know throughout the veterinary community (and we know this well here on Second Chance as the number of owners who need help skyrockets.) She has had multiple triggers to set off her genetic predisposition to autoimmune disease.
While this sounds very discouraging, we have been through this and many owners we have helped have experienced the same thing. There is great hope to recover from this and you got help quickly which was a critical advantage, good job Mom! Once this she has recovered we can help guide you through the lifestyle alterations that are necessary with our more susceptible dogs.
Your vet is surprised that for some reason her allergies seem to be abating. This is not a surprise to me. She is being given high doses of prednisone. This is similar to our body’s cortisol. When given in these high doses it suppresses the immune system, as a whole, and that also suppresses allergic reactions. It also makes arthritis feel better, and may improve digestive disorders. It is used for many of these kinds of conditions. So it makes perfect sense that she suddenly has no allergy symptoms. Why your vet doesn’t understand this, I can’t be sure. Never-the-less, when you begin to decrease this drug, you will see the allergic symptoms return.
One drug that is commonly used to treat AIHA IMHA is cyclosporine or the brand name Atopica. This drug is marketed for canine allergies but it is used “off label” for the serious autoimmune destruction of red blood cells. You might as your vet if you can add this drug into your treatment protocol, as is commonly done, and then slowly decrease the prednisone. The Atopica will be effective at the suppression of a certain type of white blood cell that is responsible for the AIHA as well as the allergies.
Once she has improved you could go to a lower maintenance dose of Atopica to treat the allergies. Many dogs use this lower dose for this.
Vally can help you set up a medication chart, which she is a master at. We can both help you with her diet and how to evaluate the side effects of the drugs vs the disease. In some cases the drugs make the dog feel worse than the disease!
I would like to see her CBC and chem screen to help you understand what those numbers mean. Please upload the latest test results on the Urgent Advice page, see the menu items at the top of the page.
What questions can I answer for you?
my best, Patrice
Andrea,
This is an interesting observation.
I have an idea that you might run by your vet. Some dogs can contract Giardia and become this sick from that parasite. This is a more difficult condition to test for and treat. If they did not specifically test for it, they might not realize that it exists. Giardia can develop a cystic behavior in the intestines and may not pass into the feces continually, thus the vet may not see any visual indication of Giardia.
https://vcahospitals.com/know-your-pet/giardia-in-dogs
“A routine fecal flotation test may fail to detect these tiny cysts, which are shed inconsistently in the feces, and which often require a special zinc sulfate flotation solution for detection. ”
“The most common drugs used to kill Giardia are fenbendazole and metronidazole. These drugs are normally given for three to ten days to treat giardiasis. Both drugs may be given in combination if necessary. ”
Giardia was quite common where I hiked in the late 70’s and I did contract it. Some hikers described it as the worst pain they had ever experienced.
Since we can’t be for sure, it would be a wise test to run at this point.
my best, patrice
Hi Deb and Todd,
I was out of town last week so I have missed a lot of your discussion.
First, Dr. Dodds Liver Cleansing Diet is right on our website. Go to this page and click on her picture with Cleansing Diet. This will open a document in a small window, if you click the expansion arrow you will get the full pdf document. You can print and save this from here. It is described in detail.
https://www.secondchanceaihadogs.com/nutrition-resources
The concept behind this diet, especially for dogs that have AIHA and IMHA, but really for all dogs that are quite ill, is that foods that contain red blood cells, when digested, release the contents of red blood cells into the digestive tract. The elements of red blood cells then have to be processed by the liver and also the kidneys. Livers under stress due to prednisone or other medications will be further stressed trying to process this material. Removing meats that contain red blood cells from the diet simplifies the work of the liver.
The liver is highly regenerative and with some help can recover fine as the drugs are removed, provided there was no organic disease prior to this. Alkaline phosphatase and alanine aminotransferase are enzymes released usually by the liver when it is under stress and there is cellular death of the liver. This is not always the case but usually with prednisone this is the cause. I have seen extremely high values of these two enzymes in dogs on prednisone. Chance’s were sky high, frightening even Dr. Dodds. After all the things he went through, in the end his values returned to near normal.
I know this is extremely difficult, how far do you take the treatments? My goal has always been to encourage owners to become immediately proactive in contacting Dr. Dodds and getting on the correct protocols ASAP. The longer a dog must endure with treatments that are not effective, the sicker they become. So moving quickly maintains their general overall health so they can muster the strength to recover. Trying to pull a highly deconditioned dog out of these conditions is really tough.
We were at that point with Chance in the late spring of 2007. He was hardly able to walk, potty and he was a shell of his original brassy Giant Schnauzer behavior. One night I came home from work around midnight and I took him out to pee, just across the street to the fire hydrant. He laid down in the street and would not get up. I was hysterical, trying to roll him onto a blanket and pull him back up the driveway. Finally I woke Mark up and he came out and carried him in.
The next day I called my pet sitter, who is a vet tech, to come over and help me make a decision. We sat on the deck in fine weather talking. Chance was laying there quietly. Suddenly a rogue squirrel showed up at the feeder. He got up, scurried down the steps and made a good effort at trotting over to the feeder to chase the squirrel, giving a good woof.
Sue turned to me and said, “Patrice I see sick dogs all day long. Chance is nowhere as sick as any of these dogs. Don’t give up yet, he’s not that sick.” So a friend had recommended Dr. Dodds to me. It was 2007 and I had never heard of her. I thought how could a vet all the way across the country be interested in helping me with Chance? Well I screwed up my courage and called her. As I was leaving a message, she picked up the phone breathlessly and started asking me questions, rapid fire.
Within a week he was on her protocol. Withing 4 weeks he had turned the corner. My vet wholeheartedly agreed with Dr. Dodds protocol and was a significant help in monitoring him and administering tests and other care. It took many months for him to recover. It was nearly a year before he looked really healthy. But inside he was getting better.
Remember that the drugs are harsh, they cause all kinds of awful side effects that can seem worse than the problem you are treating. Don’t confuse those side effects with not getting better inside. The rear leg weakness is extremely common and it does go away, almost, but not quite. Chance was weak in the rear end and so were many other dogs that were treated. But that did not stop him. Rear end limbs tend to supply a kind of rudder for balance but not contribute so much to the power of the walk. Thus you see dogs moving fine with one rear leg.
Mixing slippery elm into food is not a good thing to do. By it’s very nature SE seals to the gastrointestinal wall creating a barrier to absorption of all food, vitamins and medications. By giving it this way it has been decreasing nutrition and the medication significantly. It should be given away from all food and medication at least with 2 hours or more on either side. I gave Denamarin on an overnight fast to ensure a long time in contact with any potential ulcers and no risk of malabsorption of food, vitamins and meds. This supplement decreased his liver enzymes incredibly fast. I highly recommend it. Slipper elm is fine for dogs not quite so sick, but when it comes to a dog that is critically ill it is very important to decrease those enzymes quickly.
I am not sure what more I can help you with at this point, direct me as to where you want to go with this.
my best, patrice
Deb,
The early days of manufacturing cyclosporine were difficult and there were two processes. One process led to a less bioavailable and stable dose, which could have led to a patient rejecting their transplanted heart! The newer process is far more stable and bioavailable. There is no longer a need to worry about the dosage variability in any form of atopica or generic cyclosporin sold for dogs, it is highly stable and the processes are all the same now. There is no need to monitor the blood concentration on Dr. Dodds protocol, she is giving a 2 day drug holiday when she pulse doses!
Deb,
What is happening to Charlie is not the same conditions as IMHA or AIHA.
Spelled out, Immune mediated hemolytic anemia and autoimmune hemolytic anemia, you see a common word: hemolytic. Hemolysis means the destruction or rupturing of a red blood cell.
Anemia is a shortage of red blood cells that leads to poor oxygen delivery to body tissues. So anemia is not the disease, it is the symptom of poor body oxygenation due to the loss of red blood cells. So there could also be a state of anemia if a dog was in a serious car accident or was bleeding during a surgery.
Mediated means assisted or caused by.
The other describing terms, immune and autoimmune, refer to the body’s protective system and autoimmune means attack on “self.” So autoimmune or immune mediated hemolysis means the destruction of red blood cells in circulation.
Hemolytic anemia leads to many RBC being destroyed in the blood vessels, scattering debris into the blood and plasma, rapidly altering the homeostasis of the circulatory system. This can lead to dangerous clotting and organ failure. That is why autoimmune or immune mediated hemolytic anemia are so very serious and why those conditions are considered an emergency.
So all these words together mean the destruction of red blood cells as caused or mediated by the immune system. The difference is that auto tends to be considered a primary cause or the cause is unknown.
Immune mediated means that there is one or more triggers activating the immune system to attack RBC. For many years all of these conditions were considered autoimmune, but now, more often vets and academics use the term immune mediated to indicate that there is some outside cause for the immune system to go haywire. They just need to find those causes.
Let’s look at an easy to understand immune mediated trigger. Tick diseases insert some form of bacteria or spirochete into the body. Sometimes these insert themselves inside the red blood cell so they can reproduce and multiply. The immune system sees these invaders inside the RBC and decides that it must attack them. But it also destroys the red blood cells! This is immune mediated hemolytic anemia. If you treat the tick disease by giving doxycycline, you hopefully can stop the hemolytic anemia.
There are many many triggers and usually in dogs there will be several triggers that combine to set off the immune mediated anemia. That’s why a comprehensive history is so critical. Often these dogs tend to have something in their genetic makeup that make them more prone to expressing autoimmune disease. Environmental triggers contribute along with things like viruses, parasites, sex hormones. All stirred up by “stress” which is the biggest contributor to autoimmune disease.
So hopefully now you understand the terms AIHA and IMHA.
So let’s look at bone marrow failure. There are various terminologies that describe more specifically what and where the actual failures are, but for now just think of this as the bone marrow is unable for some reason to send out new RBC to the body’s blood circulatory system.
At some point in his life Charlie was quite able to make new RBC. But sometime earlier this year he began to have trouble with this process. Why and when?
Jean Dodds has been studying and treating this bone marrow failure in dogs for more than 30 years. While academics and other researchers can point to multiple conditions that can cause bone marrow failure, Dr. Dodds has seen first hand that most dogs she has treated with this condition have a similar autoimmune attack WITHIN the bone marrow that leads to the destruction of precursor cells in the marrow. This is maturation arrest. In fact she knows that this is quite common in dogs.
But yet many vets in the world do not understand this. There can be other rarer causes of this as researchers and vets will point out, but for sure while I have seen this many many times in the dogs that need help on our website, I have very rarely seen any of these more obscure causes. And I have seen vets fumble with this condition, not understanding it well and unable to think clearly about the application of appropriate protocols. They get lost in doing too many tests and continue to look for an elusive cause. This most especially happens at teaching universities where odd cases make for great research and interesting papers. The more testing the merrier, at great expense to the owner. I have come to the conclusion that any qualified vet, and especially those with a background of curiosity and dedication to the field, develop amazing protocols that really save lives. My country vet is far more advanced in her treatments than some of these multi-million dollar vet hospitals.
For Chance his genetic background definitely contributed. First was the expression of complex canine atophy at a young age (canine inhaled allergies) that resulted in serious skin problems. We learned that he had gradually developed hypothyroidism, another very serious condition that contributes to bone marrow failure. He also had a digestive disorder and inherited the inability to properly digest and utilize vitamin B12. He developed a condition called extramedullary hematopoiesis, the making of blood in another organ other than the bone marrow. This growth was on his spleen. We commonly make blood in utero with the spleen before we fully develop our bone marrow. So the body has a place to fall back on to make blood somewhere else.
The bone marrow is a living tissue and it is extremely active our whole life, each day, making new cells. It never stops and it controls the amount of RBC it needs to make by monitoring the body signals when tissues complain they are not getting enough oxygen.
This graphic is a simplified look at the multiple steps that are involved in the maturation of all the cell types that are created in the bone marrow. There are many steps involved that are not shown.
https://www.secondchanceaihadogs.com/AIHA_Terms/hsc-hematopoietic-stem-cells
So at some point in Charlie’s life he slowly stopped making RBC even when the body demanded it. All the RBC that he made in the last 120 days that were in circulation were still ok, they had been made properly, so you didn’t notice he was slowly becoming anemic. It is a very gradual loss of RBC as they age out, a little each day, but not enough to be a dramatic change.
So I hope you can begin to understand that this condition is totally different than hemolytic anemia. It isn’t dangerous, there are no risks of clots. The integrity of the blood vessels is still ok, there isn’t debris in circulation. It’s a very slow loss over time.
But yet profound bone marrow failure is far more serious and deadly because if you can’t figure out how to help your dog make RBC again, they will certainly become extremely ill and maybe even die.
So now I hope you understand that this destruction is going on inside the bone marrow and that is a very isolated part of the body. How to stop the damage?
This is how Dr. Dodds began to study canine hematology. Her first job out of veterinary college included a position with NYS where she was in charge of the human blood supply at a time when AIDs and blood safety were becoming important. She decided, as a veterinarian doctor with a specialty in hematology, that she would change her career and begin providing blood services for dogs. There was no looking back.
She began seeing these dogs with the same symptoms, profound bone marrow failure at the precursor cell stage. She calls them pluripotent stem cells (master cells.) She was watching with interest the new heart transplant surgeries and the treatments human doctors were developing to prevent rejection of the organ. Because prednisone had so many terrible side effects they were looking for some other drug to use. This is when cyclosporine was first introduced. It’s main function was to stop the activity of the killer T-cells of the immune system from attacking the new transplanted organ. It is still used today.
Dr. Dodds picked up on this concept for dogs. She rightly thought, why not try using cyclosporine in dogs to stop the immune system from destroying red blood cells or killing off pluripotent stem cells! And it worked extremely well. She eventually developed a pulse dosing protocol (you can find this in that protocol I linked you to) for the cyclosporine. After a while veterinary pharmaceuticals decided to do trials with cyclo, but for canine allergies, not autoimmune disease. They discovered that dogs actually did fabulously with cyclo and so they marketed it as Atopic, for atophic allergies.
So that is the key to stopping the destruction in the bone marrow, high loading doses of cyclosporine, in Monday through Friday (Saturday and Sunday off) pulse dosing for approximately 3-5 week cycles. The doses are high, it wasn’t exactly pleasant for Chance, but I had no choice. He was going to die if I didn’t do something and Dr. Dodds was such a famous vet that I felt compelled to give this a go. Within 4 weeks, my vet came into the exam room with the CBC and a smile on her face. Chance began to become regenerative again. It was tiny but it showed me immediately that he was going to live. His poor body was in a terrible state from months of high dose prednisone, but Jean never gave up helping me and my vets were just delighted to be working with her. They were just stunned that this protocol worked so well.
It took Chance a long time to recover his body condition. But inside his body it was beginning to heal and he acted like he felt better. I didn’t care about the cost of his medications. I could see he was going to live.
I am unhappy that you were talked out of the cyclosporine because of the cost. I hope you will reconsider this decision. I think it is critical to gradually reduce the prednisone and aza and switch over to cyclosporine as the main immunosuppressive drug.
Dr. Dodds will look at your lab workups and will probably recommend her protocol. She may have more advice about the medications you are currently using.
My experience is that aza can lead to profound bone marrow suppression over time and thus it could actually be part of the reason why the bone marrow can’t respond any more. Aza is a chemotherapy drug. It is designed to suppress and stop the reproduction of rapidly growing cells. Great if you are fighting cancer. But our skin and our bone marrow consist of rapidly growing cells! From start to finish you can push out new RBC in about 7 days. White blood cells and platelets have an even shorter growth process.
I truly hope you also understand why I don’t recommend a bone marrow biopsy. You already know that Charlie is not making RBC and there is a pretty good chance that it is autoimmune destruction of the pluripotent stem cells. The test will only confirm what you already know, he’s not making blood, it will not help change the treatment protocol. The test requires anesthesia and sample collection from the shoulder or hip that can be quite invasive. It will leave Charlie sore and struggling to recover from the anesthesia. Chance had this done and I regretted it, it told me nothing and it didn’t improve his treatment protocol. It was time for me to see another vet.
Put the money you save by not having that test towards future blood transfusions and atopica.
my best, patrice