Forum Replies Created
Rick,
It sounds like you have researched very carefully and understand a great deal. I admire you for taking the care to do that for her. What you had go through to get her care was very difficult.
Can you say when the last good meal is that she ate? Has it only been a day or two or did you notice that she lost her appetite about a week ago when she first did not feel well? Was she ever a good eater or is this a rather new symptom? Can you pinpoint anything at all that was different that day?
However, sometimes dogs just don’t feel like eating. It’s a tough decision whether to let this go for a bit of time or to intervene. Clearly it is not ok for them to stop drinking. If you have to use a baby med syringe from the pharmacy to get her to take water then you must do that. If you can make up a little slurry of over cooked rice water (rice congee) with some sugar and a dash of salt then syringe that slowly into her cheek, all the better. I agree that the prednisone is bothering her stomach and it is far better if she is eating something with it. My vet told me to use something very smelly like fish. I had a number of things I rotated through like cream cheese, real canned cheese, liverwurst, canned sardines.
It is difficult to determine how she is reacting physiologically to her meds, due to the fact she has been on prednisone prior to now. Though you did say she was on 1mg of pred per day and that is quite a low dose. Some AIHA dogs continue on with a low dose like this for the rest of there life. Keep some notes in the kitchen so you can recall how she is behaving during the day so you can report when you next talk to the vet.
So she is now on 40mg per day? Are you splitting that BID, twice a day with food? This would be the ideal way to give this.You most definitely want to be giving her stomach protection such as Pepcid or Prilosec an hour before those meals. We can never quite know whether a dog will develop stomach ulcers, but my experience is that it is far better to just plan on that eventuality, be proactive and protect the stomach.
The sucralfate is excellent at healing any possible ulcers that may develop. It is kind of like a mucous internal “band-aid” for the esophagus and stomach. Because of that you must be careful to not give it too close to when you are giving food and medicine because they will not be absorbed properly. Timing meds can become difficult the more of them you give, but I found that giving the sucralfate on an overnight fast was the best for Chance, it had all night to work. If you cannot accommodate that then be sure to give it at least 1-2 hrs before a meal with meds or at least 3-4 hrs after.
I knew that the PCV would drop like this, it is a common occurrence. She may end up settling in a bit lower than this. There are three broad ranges of PCV values. Mild anemia is usually around 30-32 to 37%, moderate is approximately 21-30% and below that is variably considered severe. Each dog is a little different in how badly they feel at certain PCV’s. Some dogs can tolerate 8% and seem as happy as ever, other dogs are just not well off at that value. So determining a “transfusion trigger” point is a variable dependent on a combination of the actual PCV but also the clinical evaluation by the vet. However most vets would probably think of 20% as an acceptable value to consider another transfusion.
The first transfusion a dog gets is “free.” That means, unlike humans who must always be matched, a dog can take any blood type for the first transfusion without reactions. Dogs have approximately 11 different “types.” After the first transfusion a dog must be typed and matched for the next one to avoid reactions. Being in facility that is prepared to do this more complex step in an emergency is good insurance. There are different blood products available too. My vet was able to use whole blood directly from her own donor dog. The next best product is packed red blood cells. In an emergency, super washed red cells will reduce the transfusion risks significantly but the washing does reduce the number of RBC and platelets.
I always think what I would do if this were my dog. I will always be quite honest about how I feel.
So, if this were me, I would consider these first few days a period of emergency. I would find, if I could afford it, the best specialist in town. I am lucky that my own country vet is the best specialist in town, but not everyone is that lucky. If your instincts are telling you that you need to feel a bit more comfortable about a second opinion AND you think she can handle being taken to a new location, then any vet should graciously welcome a valid second opinion and may even be polite enough to refer you. This is not a straightforward case, she has complications with the Addison’s condition, that is reason enough. Never burn your bridges, be polite and thankful for the great care she has been given. You may have to go back there.
There is still a great risk for clotting emergencies right now. Please request permission to give her low dose aspirin therapy. This therapy has been researched and is an approved protocol for treating AIHA canines. A dog that has active hemolysis needs to be protected.
Yes, the accuracy of these blood tests can be variable and there are common mistakes that can result in wrong values. Some vet techs are wonderful, they take great care with their job. Seek out those techs and be sure to ask for them each time you visit. The decisions you will be making are dependent on the accuracy of these tests. You are her advocate, get what you need as politely as possible. I promise you that this will be of value.
If she is resting tonight and is not struggling, why don’t you get a few hours of sleep and then take her in early in the morning, is there someone else that can stay awake while you sleep? That is a good compromise. You will get the morning staff at their best before the rush starts.
my best
patrice
Rick,
Thank you for the complete history. This is important information.
I do not subscribe to the “old dog illness” theory. Neither does my vet. Chance, who was my inspiration for this website, was an older larger breed when he was diagnosed. What I said to my vet, before I knew what the problem was is that “he looks dumpy to me.” She firmly told me that we owners confuse how humans look as they age with how dogs age. If our dogs are kept healthy, they do not look dumpy as they age! He was not healthy at that time.
Brandy is a medium sized dog with an expected life span of up to 15 years. I am never completely satisfied with “underlying medical issues” as a complete diagnosis. In general, unless a dog is very sickly as a puppy (perhaps due to genetic deficits in a pure breed), I am not convinced of a definitive exclusive diagnosis of Addison’s Disease.
Pancreatitis is, unfortunately, a condition of equal opportunity owing to a dog’s less than hygenic eating habits. However, in most dogs, this is usually a singular event following social gatherings like holidays (too much turkey fat sneaked under the table) or food stealing as a young hungry dog (the whole turkey.) If properly taken care of at that time by a vet, most dogs usually recover from these one time events and can go back to eating a normal diet eventually, being mindful of keeping it on a lower fat side. Prednisone has been linked as a possible contributor as well.
I am not exactly sure why they prescribed multiple courses of antibiotics (unless you are referring to Metrondiazole) for this condition, but I do know the outcome of frequent antibiotics in a dog. SIBO small intestine bacterial overgrowth (good bacteria is destroyed by the antibiotic leaving room for bad bacteria to proliferate.)
The small intestine is the organ of digestion where all food is assimilated into the system as nutrients. The loss of good bacteria in the SI leads to SIBO which causes severe inflammation of this organ and malabsorption of important nutrients. The other outcome is that the colon receives a great deal of undigested food and bad bacteria plays havoc creating diarrhea, gas and perhaps even colitis.
Addison’s Disease can be known as the Great Pretender, with vague symptoms similar to other conditions. Has your vet ever done an ACTH stimulation test? This should have been done as a rule out years ago. I am surprised it took you 3 vets to find some help.
For others reading this: Addison’s disease results in basically the opposite of too much cortisol (Cushings), resulting in low levels of cortisol, and leaves a dog constantly struggling to handle stress conditions properly. Weakness, collapse, poor appetite, vomiting, diarrhea, problems regulating body temperature etc are all the vague symptoms of this condition. Because the body’s daily needs for cortisol are extremely variable, they may appear to be relatively fine, but when stressed, they may be very ill.
What is possibly an explanation for all of this is a companion condition to SIBO called Leaky gut syndrome (which could result from pancreatitis). The inflamed SI leads to leaky “spaces” in the walls of the small intestine. Undigested food, toxins, and bacteria leak into the bloodstream.
These noxious wastes can lead to allergies of the skin and respiratory system, joint pain (arthritis), irritable bowel disease, autoimmune disorders, diabetes, and many other issues related to the Pro-Inflammatory Response.
I am going to guess that there was some autoimmune component to this condition, possibly resulting in some level of destruction of the adrenal glands. If that is the case, then it is possible that Brandy has had a tendency to other autoimmune conditions as well since then (hypothyroidism?.) This can result in what is called a Pro-Inflammatory response. High levels of pro-inflammatory cytokines such as Tumor Necrosis Factor and certain interleukins result in negative changes to how the body handles “stress.”
The main player in AIHA is usually considered to be the T-cell lymphocytes. These reactive white blood cells are usually our protectors. But these killer T-cells can also lose their original instructions and begin attacking “self.” Suppressing them is sometimes the only solution to stopping the destruction. Unfortunately, the side effects of suppression on the rest of the body are quite serious.
There are other treatment protocols for Addison’s that may be more satisfactory than simply prednisone. Fludrocortisone (trade name Florinef) and a monthly injection called Percorten-V (desoxycorticosterone pivalate, DOCP) may be alternatives.
I don’t normally recommend that folks see an alternative veterinary professional but I think in Brandy’s case this would be a good consultation, once she is stable. I would also advise that you be very cautious about administering kelp. This nutrient rich supplement can contain so much iodine that it can suppress and cause thyroid dysfunction leading to hypothyroidism. Kelp supplements can contain iodine in amounts that are up to several thousand times higher than the daily tolerable upper limits for iodine (in excess of 500-1,100 mcg iodine daily). I was attending a Dr.Dodds’ seminar when she first learned that studies had shown this to be the case. Who knows what dog foods and supplements contain since they are so loosely regulated.
So the top priority is stabilizing Brandy so she can withstand the immunosuppression that is required to halt the autoimmune destruction of the red blood cells. Keeping her healthy is very important right now with lots of rest, good nutrition and very low stress. As the days go by you will be more comfortable with providing care for her. Right now, let us take on the heavy worry for you. Be kind with yourself so that Brandy feels at ease.
my best, patrice
Rick,
I have prepared two AIHA introductory videos that you may want to watch.
We also have an extensive glossary of terms.
You may want to view Our Stories, they will give you some insight into how each of our dogs was diagnosed and treated.
my best, patrice
Rick,
I am so sorry to read about Brandy. This does clearly sound like AIHA esp with the results that you have provided. Can you provide us with her age and weight please?
Dexamethasone is similar to prednisone but is usually given this way, in a much larger starting dose in hospital. Prednisone is also an immunosuppressive. Both act immediately to suppress the immune system when given in high doses.
It is common for the PCV to drop some after a transfusion. Do not worry about this right now. You are correct in thinking she may need another transfusion.
The question at this point is was there a specific trigger that started this hemolytic destruction? What tests did they do to check for triggers that might need to be treated?
At minimum they should have checked, esp at this time of year, for tick diseases. They should have asked you questions about anything that Brandy might have eaten such as rat poison or food with onions or garlic. Did Brandy recently have vaccinations or is there a chance she had a bee sting? Is she an outdoor dog? Does she go to wild areas where she might contract certain diseases like Leptospirosis? Has Brandy been a healthy dog or does she perhaps have allergies? An older dog should have a thorough check of the internal organs to look for growths. We always like to see a complete checkup.
The goal now is to stabilize Brandy and stop the destruction. She is actively regenerating new blood cells, you can see that by looking at two results you posted:
2+ Polychromasia is present. This means that there is variability in the color of some of the red blood cells. These reticulocytes, which are immature “baby” red blood cells, still contain RNA from their development stage and when viewed on a slide that has been stained with blue, show this strong variation of color. It is simply an observation that was made in the lab and is not something bad.
2+ Anisocytosis is present. This means that there is a variability in the size of some of the cells. The reticulocytes, those new baby blood cells, are larger because of the RNA inclusion. So on the blood smear they appear much larger.
An automated blood analyzer will see these variations and note them. But usually in a case like this, a competent clinic will view a blood smear under a microscope as well. We hope that your clinic takes great care in how they collect and handle blood. Please pay attention to this process as mistakes can be made that impact treatment decisions.
So now she is at home and you have been handed over the nursing care. That is pretty scary. She is very sick and she will be very tired. Give her the space to recuperate and esp today, keep the house quiet. No visitors.
Plan on making easily digestible food, a simple diet of cooked skinless chicken (saute it in a pan to make it smell good) and overcooked white rice with a little of the chicken broth will be a perfect start. She may respond to the good smells.
Make a list of all supplements she normally gets, we may need to eliminate some of them that might interfere with her treatment.
A great concern now is serious clotting. I hope they addressed this with you. If they did not you need to contact them and ask if you can put Brandy on low dose aspirin therapy immediately. The blood is not stable right now and clots can form quickly and travel. If you see any signs of difficulty breathing, sudden unsteadiness etc, please take her to the emergency clinic.
Another serious concern is stomach ulcers caused by the Prednisone. She must be on some kind of stomach protection. We usually recommend over the counter stomach acid prevention that is used for humans. You can get something like Pepcid or Prilosec. Depending on her weight she will need at least one, if not two a day, and given about an hour before meals.
On your next visit, discuss protecting the liver from the prednisone. Liver enzymes, indicating damage, will begin to elevate. The liver is processing the drug. This is normal. And the liver is regenerative. If there was no organic liver disease prior to this, the liver usually will rebound and recover once the dosage of prednisone is reduced.
You are going to see many changes, the first of which are increased hunger (hopefully!) and thirst. She will be peeing constantly. You may have to sleep downstairs with her to let her out at night. She can’t help herself, don’t be upset with her. She may pant and seem uncomfortable. This too, is a side effect of excess cortisol (prednisone) in the body. It causes the body to be on alert and prepare for stress.
Keep an eye on her stools. You may see dark stools and orange urine indicating red blood cell destruction. It is hopeful that after a few days on the prednisone the destruction will stop. But sometimes they need to increase the dose or add another drug to help do the job.
We are always here to help you, day or night. We urge you to be polite and respectful when you visit your vet’s clinic, but be mindful that you are Brandy’s advocate. You are with her constantly, your vet only sees her for about 20 min. In all cases ask politely that you be with her when she is in clinic. Stay out of the way and be quiet but make sure this happens. If you need an excuse say that you are a student and want to learn.
Ask for copies of all her records. We are able to review that bloodwork for you and explain it to you. When you have a question, ask here first. We will give you the background you need so you can discuss this intelligently with your vet. Your goal is to be a partner in her care, not sitting in the back seat.
We are always optimistic, each dog has a chance at the same positive outcome if the treatment is approached in carefully thought-out approach.
my best, patrice
Hope,
Well, I admit being surprised by the information I found. This may be pretty odd but pass this by your vet tomorrow. Merck Manuals are valid and authoritative.
Chronic Ulcerative Stomatitis
Chronic ulcerative stomatitis involves inflammation of the mucous membranes of the mouth. Signs include severe gum inflammation, receding gums in several sites, and large sores on the mouth surface near the surfaces of large teeth. The problem commonly affects Greyhounds, but it has also been seen in Maltese, Miniature Schnauzers, Labrador Retrievers, and other breeds. The characteristic feature is the contact ulcer or sore that develops where the lip contacts the tooth surface, most commonly on the inner surface of the upper lip next to the upper canine teeth. These abnormalities have also been termed “kissing ulcers” because they are found where the lips “kiss” the teeth.
The cause of this disease is an immune system dysfunction that results in an excessive inflammatory response to dental plaque. For this reason, thorough plaque control through professional cleaning and excellent home oral hygiene (including tooth brushing) may resolve the problem. Supplemental antibacterial measures, such as topical chlorhexidine rinses or gels, may be prescribed by your veterinarian. In severe cases, topical anti-inflammatory preparations may provide comfort. Discomfort caused by the ulcers can make it difficult to brush your pet’s teeth and give oral medications. If discomfort is severe and you are unable to brush the teeth, extraction of the adjacent teeth may be necessary to remove the contact surfaces on which plaque accumulates. Although extraction may aid in control of the sores, it may not completely cure the problem, as plaque grows on all surfaces in the mouth and animals can continue to develop sores.
I wouldn’t get terribly upset by this right now. There are plenty of chlorhexidine products on the market, stuff you can add to drinking water, chews, wiping pads etc. Once you talk with your vet you can probably get some samples at the vet’s office to see if it helps any.
my best
patrice
Hope,
They are probably sharing the same bacteria then, back and forth.
Chance’s staph spots were red, oozed a little yellow exudate, the hair came off in that round area and then they dried crusty. Once they cleared up the skin was hairless and shiny. Giant Schnauzers have hair not fur and their coats behave more like human hair when they are on high dose prednisone, they just lose their hair in spots.
But that is just one variation, you can see the quote above indicating that some staph looks similar to a hard pimple.
This isn’t life threatening and you will be at the vet’s soon enough. The harder part will be finding an antibiotic that he will be able to tolerate. Make sure you go over all the details about what they give you so you know what side effects to look for. Not all antibiotics are easy on dogs. Give the whole prescription, don’t stop if the skin looks better.
my best, patrice
Hope,
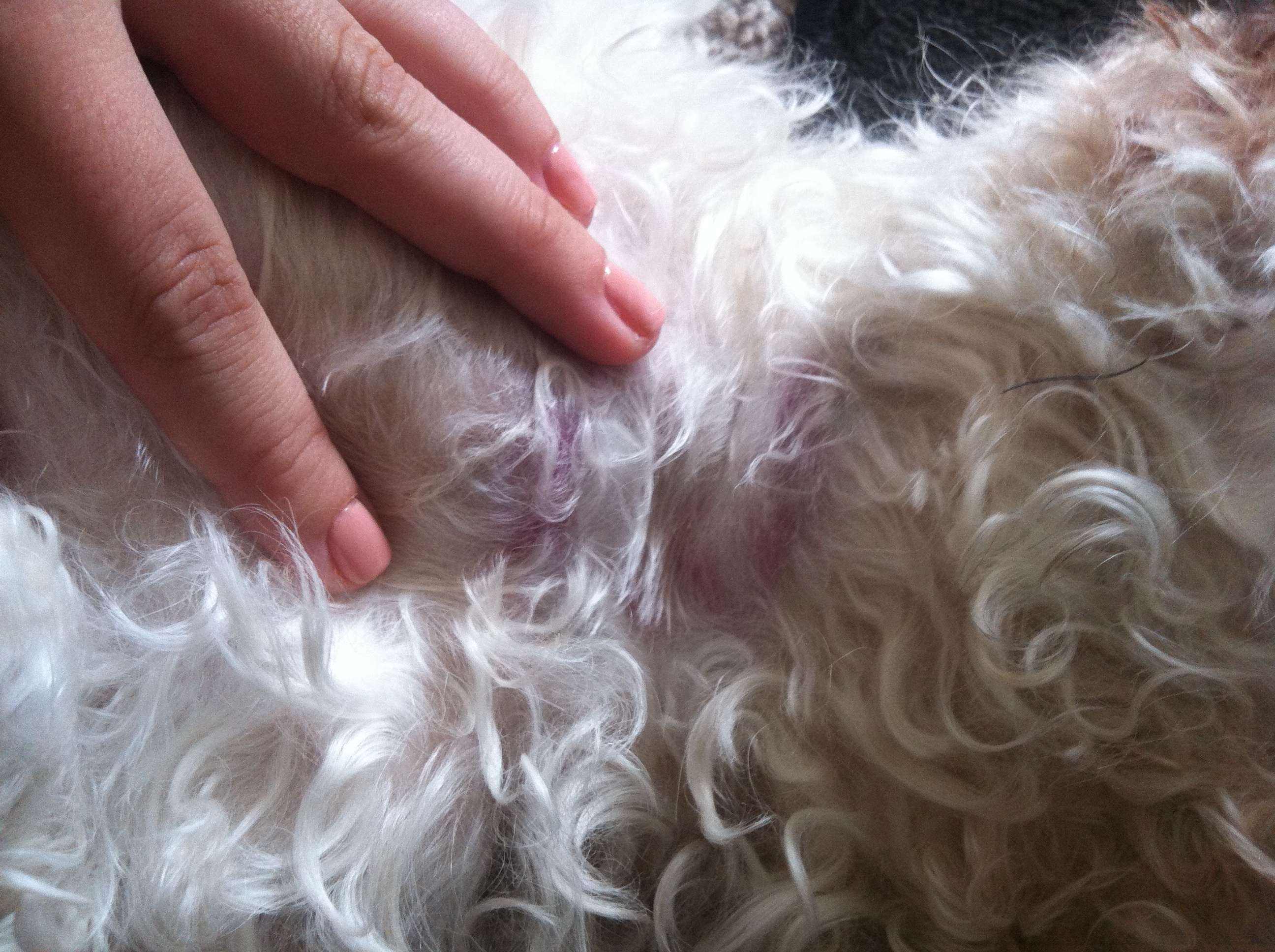
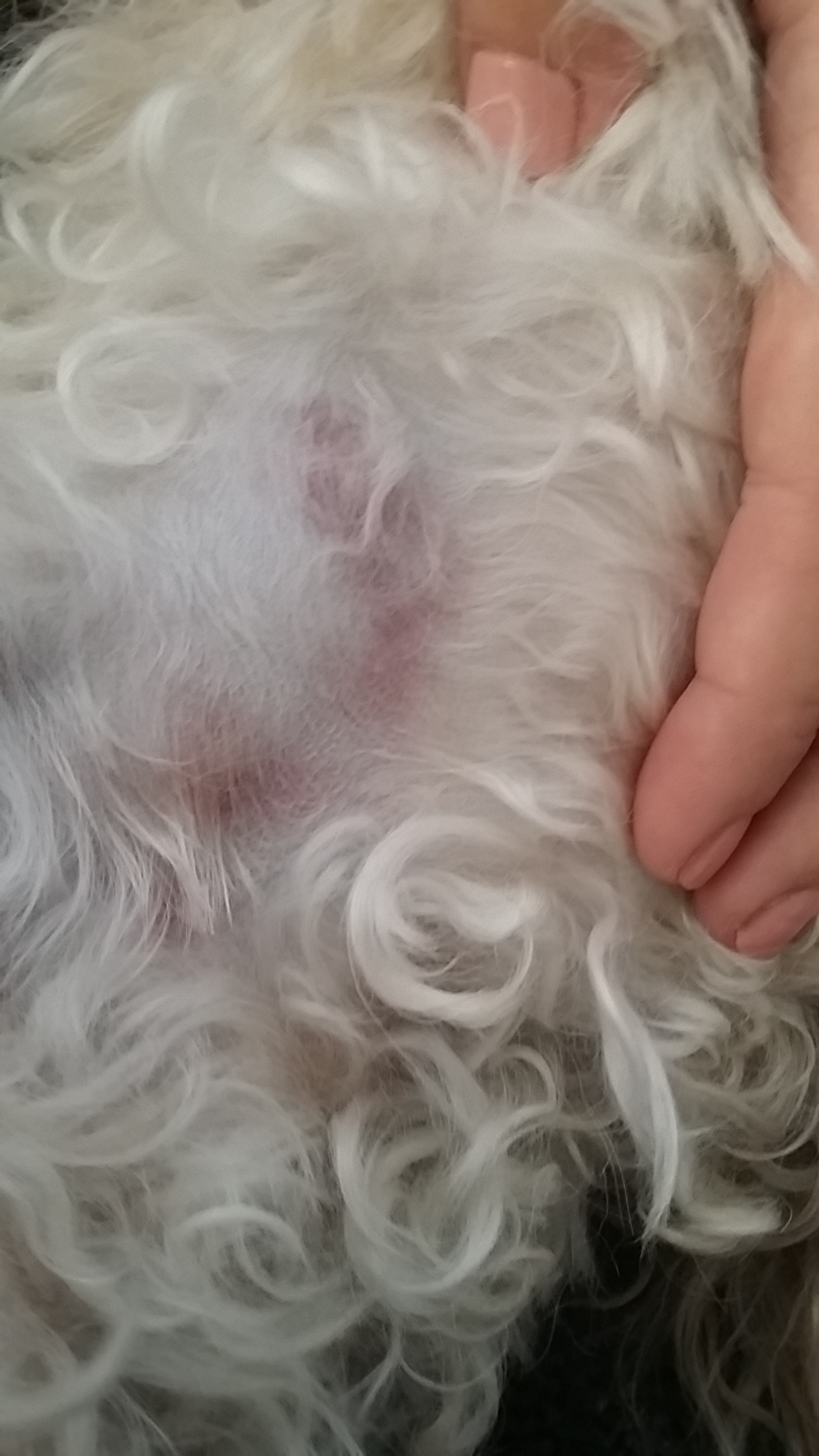
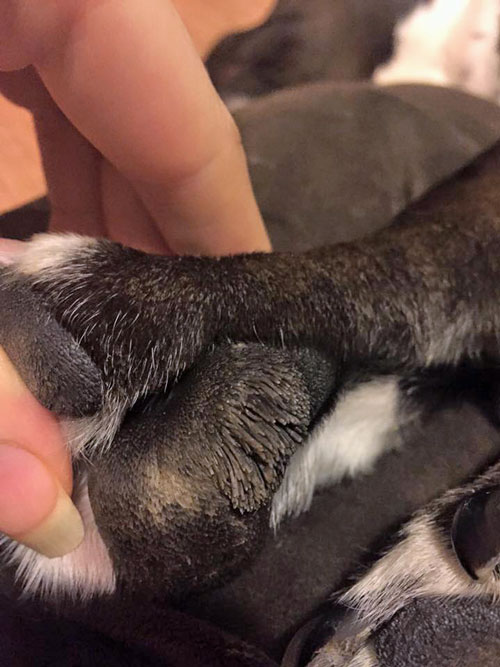
It’s a bit blurry, but I think it looks like staph.
“There are two typical Staphylococcal lesions. One type begins as a red area on the skin with a pimple-like pustule in the center. The other type is a circular, reddish area with a crusty edge and hair loss in the center. The latter can easily be confused with ringworm or yeast skin infection. Finding either of these skin patterns in a dog that is scratching is highly suggestive of Staphylococcal dermatitis.
Confirmation can be made with bacteriological cultures or skin biopsy.”
Yes, you do need to see the vet. They will probably take one look and confirm this is staph. You will be given an antibiotic.
What you can do at home. Keep everything clean. Wash the spot with gentle soap and dry it carefully. Wash your hands carefully before and after touching him to avoid spreading it around his body or to yourself. If you see other areas forming, trim the hair away and keep them clean and dry. Wash bedding carefully with hot water.
Don’t let him near family members who may also have a compromised immune system. Avoid having visitors over or other dogs.
Some strains of staph are quite mild and respond to antibiotics quickly. There is one particular strain, MRSA, that is not mild. It can become serious. Early intervention and appropriate treatment are the best approach.
I wish I could say that you should keep him from irritating the spot but that is unlikely unless you take round the clock guarding shifts to stop him. Avoid foods that might irritate the skin. If all else fails and he will just not stop bothering it you may have to put a cone on his head. Messing with it will just spread it.
my best, patrice