Forum Replies Created
Kisha,
I’ve been on a private tick discussion group since 2007 and have picked up a lot of information about tick disease. There are a few tick diseases, and one in particular, that can hide out for years and return much later with a vengeance. The dog can have a brief illness and then much later present with sudden serious symptoms that can lead to death. I am never truly convinced that it is appropriate to disregard previous tick bite history. I have helped owners whose dogs were in these last stages and it was very difficult to watch these dogs crash so quickly. The owners could not understood how a tick bite a year ago could do this. Nor did they understand that many vets fail to treat the original tick bites with the proper dose of doxycycline, or as we say, “only tickled the tick,” allowing it to hide where it couldn’t be affected by the medication.
On this page, click on Tick Borne Diseases and Dogs.
https://www.secondchanceaihadogs.com/parasite-resources/
Gil has spent years collecting and modifying this information. Click on the picture of the page to open the site in a new tab. You can read many of the pages if you wish but it might be good to start by reading her information about Erhliciosis, click on that page in the right sidebar. She discusses the three stages of the disease, the last often happening much later.
I am merely trying to encourage you to not discount further testing for tick diseases, not scare you. In a dog that has very few risk factors this is still an unknown as far as I am concerned.
The other page you may want to consult is the Test Laboratories. I recommend ProtaTek. This is all that Dr. Holland and her staff do, test for tick diseases and other like conditions. She is always willing to discuss things with a vet on the phone. The main issue comes down to the difference between a screening test (is there some indication of infection at some point in time) vs a test that measures titers (how much infection is there.) It’s not quite that simple, but when you are looking at a disease that can hide in the body you want to be able to measure “how much” not just yes or no.
When Chance was so very ill in 2007, these were the first tests I had run, I was hoping to God that it was a tick disease and we could treat it with doxycycline. It wasn’t, as Dr. Holland explained to me, the titer was extremely low and could be explained as an aberration. She’s good with these tricky lab results.
As for dry food, Dr. Dodds would be the first person to note that dry food can be tainted with dangerous microscopic molds like and fungus like Aspergillus which may cause serious illness. I would never assume any dried dog food is perfectly ok.
I would like to see a chem screen from any time during this diagnostic period, this is the test that looks at the functions of the body such as the health of the organs, blood sugar etc. I am looking for a specific reading. You will know you have done one because it can be very expensive, more so than the CBC I was able to look at. Thank you.
Perhaps you can tell me more about the actual day you felt he was ill and how he behaved when you thought this. That would be very revealing. We should try to tease this out a little bit more for your sanity.
my best
patrice
Kisha,
Pardon my delay in writing.
I’ve looked over your vet laboratory workup. My first impression is AMAZING. I will I could get this kind of workup for myself. You have a great clinic, vet, if perhaps a little overboard in expenses….
The good news is that everything is absolutely normal with the exception of the anemia, ie, the low number of red blood cells.
Your vet correctly notes that this appears to be IMHA. What they note seeing are spherocytes. If you follow the link to this glossary item that pops up when you hover over the word, you read that spherocytes are red blood cells that have a “bite” taken out of them and there is a picture of what this looks like. This is indicative of an autoimmune attack on red blood cells in circulation. So we can be pretty sure that the immune system is attacking these red blood cells.
He is wildly regenerative. This means his bone marrow is responding appropriately to the anemia in a big way by making a lot of reticulocytes. We like to see this and what we would really want to see is an end to the RBC destruction. Those reticulocyes will turn into RBC within a few days and it would be great if they could survive.
What is not clear is what the trigger is that is causing this to happen. Your vet has done some extensive diagnostic rule-outs and they all are showing no problems. So now we have to do some of our own detective work.
I am positive your vet asked you a lot of questions about his daily life, unusual events in the past month, could he get into things that might be dangerous like rat poison. Do you live where there are snakes, poisonous spiders, or perhaps near wilderness areas? Was there recent vaccinations, flea, tick or heartworm meds? Any chance that he had food that was “off?” Could he have eaten food with onions in it? The more unusual things you can think of the closer we can come to figuring out what might trigger this and what things we might be able to reverse.
The meds are all great, no worries there except that we will begin to look at the side effects that arise from high dose prednisone. You are going to see higher liver values, extra peeing, huge appetite, skin issues etc. It really affects the whole body negatively, but it is necessary right now to suppress the immune system.
We can help you with all these side effects as they begin to appear in the coming weeks.
Do you have any questions I can answer for you?
My best, Patrice
Carrie,
I am so glad to hear that Daisy is doing much better!
First, the blackish spots on the skin are side effects of the drugs and are not in any way harmful. I was giving my old girl a haircut Sunday and put her on her side so I could clipper her belly. I noticed she is developing these black patches on her skin, a sign of her great age.
As I have said many times, we go into these diseases with one dog and we come out the other side with a slightly different dog, a little more fragile considering all the treatments we had to throw at them to help them get better.
Now, as to the liver values. I would like to see the chem screen to confirm, but if you are talking about the liver values that were very high before because she was on prednisone, it would be a very good thing if they were lower.
These enzymes are markers found in the blood that are byproducts of the biochemical process in the liver of metabolizing prednisone (and some other drugs) into a usable form for the body. These byproducts indicate that liver cells were destroyed in this process. These enzymes should be normal and can even be low normal. The liver is self regenerative and recovers from many kinds of insults.
When you say rapid weight gain, describe this in more detail. Are you seeing a “dumpy looking dog” or are you talking about actually weighing her and seeing, say 5 lbs, in weight gain? So with the first, dogs that have been on prednisone lose significant muscle tone and their bodies sag, the belly looks pendulous and thus they look “dumpy.”
On the other hand increasing weight rapidly, say 5 lbs over a month, leads to me think about rapid growths internally or considerable excess fluid. So we would definitely want the vet to rule out tumor growths.
When I first took Chance in to the vets before he was diagnosed, one of the things I noticed was that his abdomen looked “dumpy” to me and asked her to feel his abdomen. This black cloud went over her face. She asked me if I would like to do an xray. I knew something was up because the original complaint had been for frequent diarrhea. In fact, there was a large growth on his spleen.
We had an ultrasound done and the specialist advised that we have a splenectomy done immediately to remove the spleen and this large growth. My own vet performed the surgery and allowed me to watch. They removed a 7lb growth plus his spleen. It was amazing in the following weeks to see how trim he looked! His waistline had returned. So my large dog was able to hide a 7lb growth in his belly and of course he weighed 7lb (plus the weight of the spleen) LESS after the surgery. So internal growths can increase their size rapidly, especially those on the spleen. It would be important to know this asap because these splenic growths can be fragile and rupture suddenly. You would not want Daisy to go through this frightening and deadly condition.
Another factor can be rapid water retention that can increase the appearance of excess weight. What kinds of conditions can lead to this? Well, in older dogs and especially dogs that have had severe anemia, they can develop heart disease like a weak mitral valve. This can lead to congestive heart failure. A symptom of this disease is the inability to remove all the excess fluid from blood in the lungs and this fluid seeps into local tissues around the lungs and heart instead of heading back to the kidneys to be removed as wastes.
Another way that fluid can increase in the body abnormally is if the liver is unable to produce enough of a certain protein called albumin that helps keeps fluid from leaking out of blood vessels. If that value is low, fluid seeps into tissues, especially around the abdomen, So there can be fluid weight gain with this condition.
So ask the vet to check for these things. I don’t have any of your past CBCs or chem screens to look at so I don’t know exactly what is happening. If you could upload the most recent on the Urgent Advice page I will look at them.
An important question to ask yourself is how is she behaving, does she seem to feel good? Perhaps she is eating more because she feels better, but that might only be a few pounds. If you notice she doesn’t seem right, then you must trust yourself to know that she is different. Dogs that are relatively healthy and active do not suddenly increase or decrease weight rapidly or in large values. Be suspicious of this and make sure the vet does some tests and evaluates her.
my best
patrice
Katherine,
I am sorry to be so late in responding, I was out of town on vacation and in an area of poor cell reception.
I know exactly what you are seeing and what is happening to Toby. The same things happened with Chance. Look at this page and scroll down to look at the photo of him on the lower right side when he was at the worse of his disease. The picture at the top of the page is one year AFTER he recovered.
https://www.secondchanceaihadogs.com/our-stories/chance/
Immunosuppressive drugs like prednisone, atopica and others reduce the numbers of certain white blood cells in the body that are responsible for the attack on red blood cells. Some drugs accomplish this via a cytotoxic (destroy the cell) action on the cells. Some antiobiotics reduce the number of bacteria by negatively impacting their growth cycle. In any case, cells that normally reproduce rapidly such as skin and digestive tract cells can be severely impacted by the actions of these drugs.
Dogs that normally have coats that consist of hair, not fur, can have serious problems during treatment for AIHA, IMHA and bone marrow failure. Chance was a Giant Schnauzer and he had hair. Your Labradoodle Toby is a mix with the Poodle breed and they also have hair not fur. So these “haired” typed dogs are really seriously impacted by the medications we use to treat them. Their coats fall out, they stop growing hair to replace, the skin dries out leaving a brillo-type coat. So Chance stopped growing hair, his elbows were open raw wounds. His coat changed to something like brillo pads.
You are clearly seeing the same things with Toby, flanks getting thin, raw elbows, his coat is blown. Eventually I was embarrassed at how bad Chance looked. I feared that people thought I was mistreating him. It was a very sad time for me and I know you must be feeling the same way. Putting a t-shirt on him in public may help you feel better.
Avoid doing any major hair cutting or grooming until you have the infections under control. The skin and the hair follicles are very delicate right now. To control the scruffy coat once he began to recover I bought some spray on conditioner from the show world called The Stuff Dog Conditioner. It smells light and isn’t greasy. I would spray this on and gently comb it through his coat.
Part of Chance’s condition was that in addition to not making red blood cells he also stopped making white blood cells. He was constantly on antibiotics to prevent him from getting opportunistic infections similar to what we hear about in very sick humans who have diseases like AIDS. His immune system was blank and he could not fight infections at all. He developed many areas of staph infection that oozed and the skin fell out. We rotated through many different types of antibiotics for him. Skin infections require a different antibiotic than would be used to treat a tick disease (doxycycline) or digestive problem (metrondiazole.) That is why vets generally like to get a skin scraping for a skin condition or a stool or urine sample to test for those conditions. This is how they pick an antibiotic.
In our daily lives, healthy humans and dogs all have staph bacteria (and many other bacteria, yeasts and viruses) on our skin normally. Our immune systems keep these populations under control and we never know that they exist. It is when we become ill that we are susceptible to these many invaders that are on and in our bodies.
So any dog taking prednisone is at high risk for expressing staph infections. Vally sent you to the link with the pictures of the way this can look. Again, staph is normally on our skin but Toby can’t defend himself from it. You must use a medication to treat this. There are some serious strains of staph infections called MRSA that can become very bad infections in dogs. Once a dog gets to this point, it can take heroic efforts to treat them.
Follow the instructions to treat staph carefully that I put in the glossary for Staph Infections. Toby is at risk of not only contracting staff but he could also be passing it off to any elderly person, immune suppressed individual or very young child in your household. Your vet probably has a favorite antibiotic to treat with. I used Cephalexin for Chance and it worked very well. His wounds stopped oozing and the skin began to heal up, the hair took longer to respond. Treatment is about 10 days.
Mites, as in demodex, sometimes called mange, are (again) on every dog (and human) in the world. However their populations are kept under control by a robust immune system. It is known that in certain breeds and certain dogs, they are born with a predisposition to expressing demodex mites in a very serious way. This genetic fault shows up as invasive infections very early in life, as puppies. These dogs sometimes require heroic treatments called dips to control. Your vet is anxious to avoid this right now because it is a serious chemical treatment. Or they are given high doses of medication to keep the populations under control.
Some of the breeds that are more susceptible are Afghan Hound, American Pit Bull Terrier, American Staffordshire Terrier, Boston Terrier, Boxer, Collie, Chihuahua, Dalmatian, Doberman Pinscher, English Bulldog, German Shepherd Dog, Great Dane, Old English Sheepdog, Pug and Shar-Pei. I don’t see the LabraDoodle on this list.
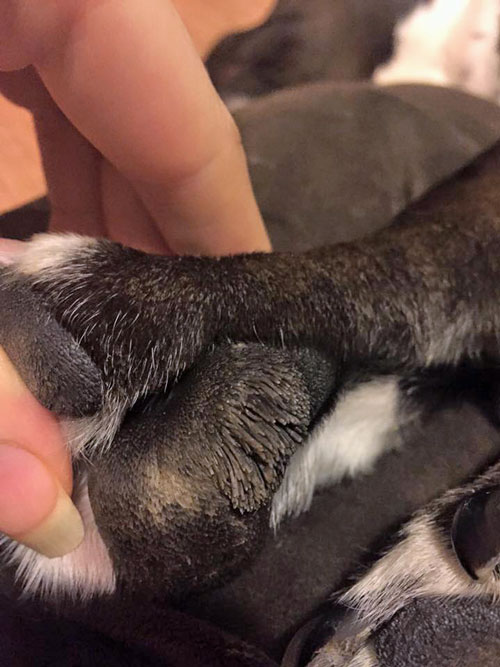
I would like to see a few pictures of Toby’s coat up close if you can. I want to figure out which parts are staph, which parts are “hair” issues and which parts are mites. Upload them on the right side bar of this page, be sure to give them a title so we know who they belong to. I won’t post these pictures publicly but I want to see them privately.
my best, patrice
Lynette,
I’ve looked over you lab results and I can say that most of it looks perfectly normal!
A few things on the chem screen that are not normal are the liver enzymes, which are high. Don’t be alarmed, this is normal to see when you have been dosing prednisone. The liver cells process the medicine and during this those cells are damaged. The liver is highly regenerative and once the dose is dropped, the liver will return to normal if there was no organic disease prior to this disease.
I also see a bit higher glucose level. Not extremely high. This can be a normal reaction under the stress involved in going to the vets and having a blood sample drawn. It can also occur if the blood is drawn too close to a recent meal. From now on make sure that Macy has fasted (with plenty of water) for about 10 hours before they draw blood. This will reduce the impact that fat and glucose from a recent meal can have on the blood sample.
Dehydration can make the HCT lower, as it is a percentage of the whole and this may be part of why you are seeing a lower value.
Finally I see that the monocytes are slightly high. These white blood cells play a role in our immune system’s response to invaders or inflammatory conditions such as infection. It’s not clear what this might be, but my guess would be a reaction to the liver enzymes. If all the white blood cells were elevated, I would be far more worried.
Many dogs that have AIHA, IMHA or bone marrow failure can tend to struggle a little in the early days of recovery as their bodies try to get back to homeostasis. You will see the PCV and the HCT wobble up and down over time. They were really sick and the body is working to get better. Small changes are insignificant and not worth getting alarmed about. Our body systems are dynamic and make adjustments constantly to get us back to normal. It is really amazing how hard our dogs work to get better.
In addition a blood sample and the subsequent CBC result is only a momentary measure in time. In fact, our HCT and other values rise and fall throughout the day in response to many factors, when we last ate, have we been sleeping or running? Are we dehydrated, stressed? If our dog is still taking some prednisone this can influence these values as well. Right now Macy has high liver values and that contributes to inflammatory stress caused by inflammatory cytokines circulating in the body.
I have seen over the years a trend in many of our recovering dogs of a slightly lower normal hematocrit. The ranges in Chance tended to be 34-37% HCT while if we did a PCV at the same time, it would be higher, say 36-39%. Right when he began to recover and he was regenerating red blood cells with gusto his HCT was around 45%. But his body settled into this perfectly normal lower HCT over time. I know this because his reticulocytes stayed at a very even .9-1-1.5% range.
Ask your vet each time to take a hand done PCV for comparison to the automated analyzer results. I think you will see something similar.
If you ever look at a series of several CBCs in the period just after recovery and you begin to see a gradual decrease in HCT combined with a continued decrease in reticulocyte values below 1% and 60,000 absolute then it is wise to carefully monitor this situation for a relapse or bone marrow failure.
Do a PCV in one week and be sure to tell me what that value is. In 2 weeks do another CBC and please ask the vet to add in the reticulocytes on this test (they are not on the current test.) In any dog that is being treated for this disease, the reticulocytes are a critical value to monitor.
Do you have any more questions?
my best, patrice
Hi Elizabeth,
Here is an AIHA Terms with our recommendations for prednisone reduction.
https://www.secondchanceaihadogs.com/AIHA_Terms/prednisone-dose-reduction/
You can see this is a relatively conservative approach that seems to help prevent sudden relapses. Not all dogs relapse, but a number of them do. We have found that these relapses further weaken an already sick dog, and though usually treatable with returning to higher doses of immunosuppressive drugs, it’s just another insult to their little bodies. A few dogs do not recover from sudden and horrific relapses.
There are some instances where a vet will put a dog on a more rapid reduction. There are cases where the dog has extremely severe side effects, such as horrendous liver values (in the range of 10-30x normal), pancreatitis or rarer cases of prednisone induced diabetes where it is urgent to halt the progression of diabetes. I urge owners to let their vet make these more rapid decreases. It’s a balance between trying to eliminate the nasty side effects and dealing with the risks involved with rapid reductions such as relapse or a severe condition called an Addisonian Crisis (read about this on the link I pasted above.)
When you reduce the prednisone to much lower immunosuppressive doses (such as 10mg day) you will reach a point where the dose is more or less equivalent to the amount of cortisol the body would make in a normal day. At this point you can begin dosing alternative days, attempting to reach a dose that is about 25-33% less OVER A FULL WEEK’S DOSAGE. (In other words don’t use the same daily dose you have been giving or even a lower dose and suddenly make it every other day, you have to make the every other day dose higher to start!) This requires a little math and is not an exact science, so don’t stress over this. You are trying to coax the shriveled adrenal glands to wake up and the every other day dose is like taking the training wheels off a tricycle.
So let’s say you went from dosing 15mg two times daily to 15mg x 66% = 10 mg two times a day.
You want to go to a once a day dose. 20mg x66% = 15mg once a day. This is best given at the start of the day when the dog needs more cortisone to supply cortisol for routine stress, the mailman needs to be barked at, there is running in the yard etc. Alternatively you could give this as 10mg in the AM and 5mg in the PM.
Now you are at a daily 15mg and you want to go to 10mg daily. This is easy, 15mgx66% = 10mg once per day in the AM.
Now you want to reduce to every other day (eod). 10×8=80mg per week. (I use an 8 day week to make the math easier.) 80mgx66% = 52.8. You can go to 50mg per week. 50mg/4 = 12.5. Make this either 15mg eod or 10 mg eod on M-W-F-Sun, dosed in the morning.
I would make these changes about every 2 weeks. Precede each change with a simple PCV at the vets to ensure there are no LARGE drops. Small fluctuations will be quite acceptable. This test should not cost you more than $20. Do not repeat a full CBC each time. If you are worried about liver enzymes during this time, ask you vet if they will do just a liver panel, not the full chemical screen.
During this time you must be alert for the side effects that are natural when reducing prednisone such as weakness and tiring easily, taken to the extreme you are worried about sudden collapse and other serious side effects that require an emergency visit to the vet.
In addition, dogs that had prior disease conditions such as arthritis or digestive problems or other autoimmune condition such as allergies will suddenly appear to get worse. The prednisone was performing antiinflammatory benefits and reducing the prednisone makes the pain worse and the allergies or the digestive symptoms worse. Some dogs just do better on a little bit of daily prednisone the rest of their lives to prevent relapses and if the secondary benefit is less joint pain or less bothersome allergic reactions, this is a very reasonable approach.
When our very ill dogs begin to get better we wonder if they will return to full good health. I can tell you from experience that we often go into these horrible diseases with one dog and come out with a slightly different dog. Their personalities usually remain intact, but they are a bit more fragile than they once were. Accept this and move forward. If giving a small amount of prednisone each day makes them feel better and they are less prone to a relapse then you are choosing quality of life for them.
Many dogs go on to live for many years after they recover. We always recommend a more carefully guarded approach to their lives. Less stress is the goal. This can be medical (such as too many vaccinations or unnecessary operations), environmental (exposure to chemicals, pollution, other dogs, other canine diseases, bad water, dangerous insects such as mosquitoes and ticks), dietary (such as feeding kibble), hormonal (if they are still intact, spay or neuter, and no puppies.) See your vet every 6 months for a checkup.
Do you have any questions about how I have explained the prednisone reductions?
my best, Patrice
Raya,
Each of us moderators helps because we know exactly how you feel.
We always feel there is hope. If you have time you can read Our Stories, look in the menu for the drop down menu items. You can read about Chance there. He has been gone a long time but I have not stopped helping owners since then. Vally has a similar story about Bingo.
We will get the photo up, my day has been busy and Vally is in Sydney, still asleep!
My best Patrice