Forum Replies Created
Heather,
I want you to know that I have looked over your blood work and I am doing some background research for you. I haven’t finished yet.
Absolutely contact Jean Dodds with this question. While I know first hand about dogs and surgical removal of the spleen, she has researcher level information about splenomegaly and removal. In general, the spleen is a really important organ to keep but if it is diseased or has a benign growth on it, removal is indicated.
What does the job of the spleen if it is removed? Well, the body is a little different without a spleen, but dogs do fairly well. Some of the jobs are picked up by other organs like the liver.
It has several important functions. The most basic is the storage and management of red blood cells in the body. It determines when RBC are too old to continue, destroys them and recycles the material. The do this primarily during rest periods.
In dogs the spleen provides an “instant transfusion” as my vet likes to tell me. It stores a lot of blood and if the dog suddenly needs it, powerful muscles squeeze most of the blood back into circulation.
On the immune side, the spleen makes certain WBC that are protective against invaders and works closely with the rest of the immune system to protect us. So the one major ability we have, to fight babesiosis (tick disease) is taken away when we remove the spleen. That leaves humans and dogs vulnerable.
The bigger question now-a-days is WHY has it become enlarged? Is it working on fighting something? Your blood tests show some kind of battle going on against some kind of invader like an infection or perhaps some kind of tumor. There are values that are out of their normal range that indicates “anemia of chronic disease.” But exactly what is it? This kind of anemia will smolder along, keeping the PCV around the mid 20’s for a very long time until the condition is resolved in some way.
One value that is indicative of a problem is the slightly low blood calcium. This really has nothing to do with dietary deficiency but is an important element in our ability to perform things like muscle contractions. It is also important to help blood clot and to make sure our blood stays at a certain thickness so it stays in the blood vessel. When calcium is low, there are a number of things that can be causing the problem, such as kidney disease (the bun/creatinine ratio is high), pancreatitits, hypoparathyroidism, or muscle breakdown such that occurs when taking prednisone.
The CPK,Creatine Phosphokinase, is high and this is indicative of muscle tissue damage. Where is this happening? I’ll take a guess and say that you need to think about two things, one is to make sure that they have done a urinalysis to check the kidney function and the other is to do this test: cPLI. This is Pancreatic Lipase Immunoreactivity, a specific lipase found only in canine pancreatic tissue. Let’s find out if one of these two is the chronic condition that is causing this anemia of chronic disease. These tests are relatively easy to do and may somewhat expensive, they are nowhere as invasive as removing the spleen would be.
The only caution is that if there is a growth on the spleen, it could rupture leading to severe pain and probably death. If she has already had an ultrasound and they ruled this out completely, then don’t worry about this.
So get these two tests done, ask about the lowish calcium leveland the high cPK test result. Then contact Dr. Dodds via her consultation and ask her point blank if you should let the vet remove the spleen.
my best
patrice
Hi Janie,
I am sorry to read this. The details are sketchy so it’s hard to say what exactly is going on. It would be helpful to see the blood work the vet did to determine this diagnosis. You can upload these on our Urgent Advice page.
AIHA and IMHA are relatively complex conditions that result from a series of triggers that “influence” the immune system to “fail to tolerate self.” This simply means that the immune system attacks the red blood cells as though they were invaders. But these triggers can be different from dog to dog and there can be multiple triggers! Some breeds are genetically susceptible and experience it more than other breeds. Common general triggers are stress, hormones, viruses, vaccine reactions, environmental influences. Under those categories you would find things like tick disease, tumors, infections, over vaccination, chemical and pesticide exposure, snake or spider bites, the list is extensive. The more triggers together, the more influential they are in leading to IMHA AIHA.
Sometimes there is an outside influence or a group of influences that can be identified as directly related to leading the autoimmune attack on the red blood cells. For instance if a dog is bitten by a tick and gets a certain tick disease that hides inside the red blood cells, the immune system will begin attacking the RBC to get at the tick disease. In a case like this treating the dog with a certain antibiotic will eliminate the tick disease from the body and eventually the dog will get well again. So treatable triggers are important to identify.
You clearly are aware of tick diseases, you gave her the Lyme vaccination. I am somewhat unsure about this vaccine, there can be some problems with it. Look on this page.
https://www.secondchanceaihadogs.com/vaccine-resources/
for this article and click on it:
Dr. Dodds Canine Non-Core Vaccines
She discusses the Lyme vaccine in this article.
Lyme vaccine is not usually directly related to triggering AIHA IMHA, but rather some dogs can express symptoms of Lyme as though they actually have it. Those early symptoms in dogs usually begin with some kind of shifting lameness, an overall malaise, neurological symptoms like facial nerve paralysis or changes in the iris of the eye, extreme kidney failure can happen quickly if the Lyme spirochete invades the kidneys. So Lyme is a nasty disease but doesn’t usually influence blood integrity.
Back to what you asked. Prednisone and its much more powerful kin dexamethasone can completely suppress the immune system quickly if given in high doses. That is why all of us moderators know that prednisone is a life saving drug, it works quickly to stop the destruction of red blood cells. But how about 5 days out, 10 days out, one month out? There are extreme side effects of high dose prednisone over time, that can make a dog feel very sick.
So it would be preferable to actually figure out why she is destroying red blood cells and treat that if possible. A CBC is a great tool to examine some important details. An oral history is incredibly important. A lot of owners skip over the details and if I coax them to tell me more then suddenly we find out some amazing tidbit that is treatable.
When I read your description of her the next morning I thought how this seemed similar to a condition called Addison’s Disease, often called the “great pretender.” Hard to diagnose but a key element is that it always improves with dosing with prednisone (though there are far more appropriate drugs that are used to treat it long term.)
If you are unable or unwilling to look into this further with your vet, you could continue to treat with prednisone but eventually those side effects are going to impact her quality of life. I would not quickly reduce this high dose, it isn’t good to do that in any circumstance, human or dog, and can actually lead to a drug induced Addison’s Disease. Vets use prednisone all the time and they have certain protocols for how to safely reduce the dosage. You can read what I have recommended about reducing prednisone, based on our experience with dogs that have been under treatment for AIHA IMHA.
https://www.secondchanceaihadogs.com/AIHA_Terms/prednisone-dose-reduction/
Dogs certainly don’t know why they are sick, but they are aware when they don’t feel good. They count on their humans to care for them for everything from shelter to food to vet care. Your vet can help you make these important decisions about how to care for her going forward.
I can answer any questions you have for me,
my best
patrice
Alberto,
It is quite common for ticks to carry multiple tick diseases. If a tick is carrying babesiosis, they are more likely to be also carrying Lyme, ehrlichiosis, anaplasmosis and other less well known diseases. These diseases can all have serious effects on blood integrity. They can also affect other organs, even cause neurological signs. There is not one body system that remains unaffected by tick disease.
I have been trying to explain that once a dog contracts babesiosis they dog will always carry that infection. The spleen will continue to attempt to control it but illnesses or other stresses will reduce the body’s ability to fight the babesiosis. It has not been eliminated from the body. I have added another article that you can read titled An Unusual Form of Canine Babesiosis: go to this page and click on the last item on the page.
https://www.secondchanceaihadogs.com/canine-disease-resources/
There would definitely be an inflammatory response by the body during this battle with babesiosis. This response is not the cause of the IMHA, the inflammatory response is the body’s attempt to get rid of the foreign invaders. Our bodies respond like this whenever we are sick, if we get the flu (a virus) we ache all over and get a fever. The body responds like this to tumors, infections, damage to organs, stress.
Most importantly the prednisone actually mimics the behavior of our own cortisol which is released during stress. But we are giving it in much higher doses than the body can handle. This created a constant state of “fight or flight” and severely impacts every body system and organ. You should expect higher liver enzymes. Skye will be peeing more, hungrier, body condition will change.
Having been on a tick forum for 10 years I have seen many cases of dogs having tick disease that leads to IMHA, immune mediated hemolytic anemia. This is called a secondary form of IMHA. The immune system is being “mediated” to damage the red blood cells. I explained this in my previous post.
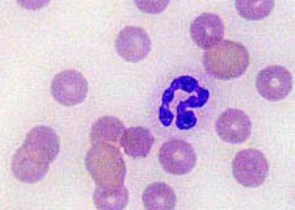
The body’s immune system senses the protozoa in the red blood cell and lyses (destroys it) to get to the invader. (I posted a picture of what the protozoa looks like inside the RBC) In the spleen the same thing is happening, the immune functions of the spleen cause it to attack the red blood cells containing the protozoa and lyse the cells. Thus there has been hemolytic anemia that is mediated by the body’s own immune system. You are worried about the platelets and that is just another similar attack by the immune system. It is not unusual and was to be expected. I believe that there is more than just one tick disease infection in Skye.
It is always a very tricky treatment protocol to treat both the tick disease and the autoimmune attack. On one hand, you want the immune system to attack the foreign invader to destroy it so you DO want immunity to be robust and very active. If the immune system isn’t successful the dog will die from the serious attack by these tick diseases.
On the other hand you don’t want the immune system to be destroying red blood cells and platelets (and even white blood cells) because that will eventually kill the dog.
So treatment is very complex. The vet must attempt to suppress the immune system enough so that it will stop destroying RBC. So the treatment is prednisone, cyclosporine, both immunosuppressive drugs. But you also want the spleen’s immunity and the body’s immunity to fight the tick disease.
So the goal has to be to use both immunosuppressives and antibiotics (like doxycycline) at the same time. It’s an extremely difficult balancing act. It is a contradictory treatment protocol and fraught with difficulties.
The expected side effects of the prednisone are severe esophageal and stomach ulcers such as you describe. The vet should have been prescribing Skye stomach protection like pepcid and should also be prescribing something to heal ulcers such as sucralfate.
You don’t need to do biopsies on this poor guy, he is too ill for this right now. He has some form of colitis or irritable bowel syndrome. Please go to this websites and read about how to treat these conditions.
http://www.marvistavet.com/colitis.pml
http://www.marvistavet.com/inflammatory-bowel-disease.pml
Mary’s site has a lot of information about what you can do at home to treat this:
http://www.dogaware.com/health/digestive.html
One product that Mary recommends it Bertes Digestion Blend
https://b-naturals.com/by-type-c-22/digestion-aids-c-22_15/bertes-digestion-blend-1-lb-p-101.html
This can be used in conjunction with this supplement FoodScience of Vermont Superior Enzymes, Digestive Health Support:
https://www.amazon.com/FoodScience-Vermont-Superior-Enzymes-Digestive/dp/B000BNX17U
You can use both or one. I recommend this for now to make him more comfortable
If you are home feeding him now I am going to recommend you begin making his meals for him using Dr. Dodds liver cleansing diet. Go this page
https://www.secondchanceaihadogs.com/nutrition-resources/
and click on the first item with a picture of Dr. Dodds. It will open a pdf with the complete diet and how to prepare it at home. Hundreds of thousands of dog owners around the world have successfully used this diet during these treatment protocols you are on right now. Do not change it in any way right now, prepare exactly as she describes.
Please try to find out the genus of the babesiosis. This is important information that will help you treat this going forward.
Please discuss the risks of DIC disseminated intravascular coagulation with your vet.
my best, patrice
Alberto,
Sorry for the delay in getting back to you.
Needless to say that this is a complicated diagnosis and treatment, it’s not straightforward because there is a diagnosis of babesiosis. As I pointed out before, the spleen is the active defender against this tick disease. The vet can assist it, and has done a good job at doing that, but when it comes down to the future prognosis Skye’s spleen will continue to protect him from babesiosis. Most veterinary literature notes that stress can tip the balance and the babesiosis will take advantage of that.
Babesia parasitizes the red blood cells of dogs. It would be helpful to know the exact genus of the babesiosis because there are many and they are different from one location to another. Canine Babesia are classified into large and small forms, with worldwide distribution. “Improved PCR techniques allow for better definition of these parasites.”
“B. canis (plus an unnamed, large Babesia sp.) in the USA (large Babesia). Three subspecies of B. canis exist: B. canis vogeli, B. canis canis and B. canis rossi. These three subspecies are genetically distinct, transmitted by different vectors and differ widely in pathogenicity and geographic distribution. B. gibsoni and B. annae (small Babesia) have been documented to infect dogs.”
“Babesia canis vogeli is the least pathogenic and occurs in France, Australia, Japan, Brazil, South Africa and the USA and usually causes mild disease in adult dogs, but severe disease in some puppies.”
“Babesia canis canis is widespread in Europe (and affects more than 400,000 dogs per year in France alone) and Asia and is of intermediate pathogenicity.”
“Babesia canis rossi occurs predominantly in southern Africa and is ostensibly the most virulent of the subspecies.”
“The smaller parasite, B. gibsoni, occurs principally in the Middle East, southern Asia, Japan, North Africa, South America and is an emerging infectious disease in the USA, as well as having been detected lately in Italy and Australia. Babesia annae has been found to be endemic in dogs in northwest Spain.”
Overall, looking at the latest lab report, Skye has moderate to mild anemia. That means it’s not so severe as to be life threatening and just anemic enough to make him feel pretty lousy.
One item on the report indicates a large number of segmented neutrophils. These are the WBC that are responsible for fighting infection or when the body is under stress.
Lymphocytes are at the low normal level, which is a goal when treating with cyclopsorine. They are generally the WBC that is responsible for autoimmune activity against “self.” We call these killer T-cells or cytotoxic cells. When they are immature they receive instructions from the immune system to assist in defending the body against invaders. They sometimes misunderstand those instructions and begin attacking the body. I like to say that they have gone “rogue.”
Platelets have decreased and are now below the normal range. You used the term “piastins” and I think that is what you were trying to write? I find this troubling because they are the helpers that repair internal bleeding. They arrive at a location in blood vessels that are signaling damage to the wall of the vessel and begin to help clot the wound. Without sufficient platelets internal bleeding in vessels can become erratic.
In order to understand why I am concerned we need to look at how babesiosis infects and reproduces. Once the tick has passed the disease to the dog, these protozoal parasites seek out RBC and infect the cell in order to reproduce. Once they are successful, they destroy (hemolysis) that RBC so that they can travel and infect more RBC, this is intravascular hemolysis, destruction of RBC in the vessels. Meanwhile the spleen is also busy seeking out and destroying RBC that contain the protozoa, this is called extravascular hemolysis, outside the vessels. Inside the spleen the immune system attacks those protozoa they find and destroys them.
Also in the blood vessels the protozoa can cause microthrombi by collecting within blood vessels. This can result in coagulation abnormalities. This is where the platelets come in. They are part of a complex process of wound healing. The body senses the abnormal clotting and attempts to stop this from happening. This process is called the clotting cascade. Fibrin, clotting factors and other elements are called to action to begin the clotting. But at some point if there are too many locations and not enough platelets and the clotting factors are used up the body begins frantically trying to lay down fibrin everywhere at one. This will create a condition called DIC disseminated intravascular coagulation that can happen suddenly and be very dangerous for the patient. Once this is triggered it is an emergency and a team of vets and techs must attempt to stop this process in clinic.
In some dogs being treated for AIHA IMHA the vet will prescribe low dose aspirin to block some of this action, other clinics use a heparin or other anticlotting agent. It is important for you to discuss this with your vet now. We do not want Skye to have an improper clotting incident. If you use the term DIC they will understand what you are concerned about.
I need to stop for now, but will continue later.
my best
patrice
Raya,
I wrote this guideline about decreasing prednisone. Perhaps something I have written will help you here? Ask me questions after you have read this.
https://www.secondchanceaihadogs.com/AIHA_Terms/prednisone-dose-reduction/
my best, patrice
Kisha,
Thank you for the update and the chem screen!
The chem screen is completely normal. There are no values that are low normal or high normal. The value I wanted to check is globulin. Dogs unable to effectively fight ehrlichiosis in the early days of infection can become chronically infected. In that case we would have seen elevated globulin levels in the blood, which we don’t.
In addition, dosing with doxycycline can be prophylactic. This means that there was never a diagnosis or sign of tick disease but that there was the potential for exposure. So dosing with doxy “just in case” is often a very good approach with tick diseases. My vet is very much in agreement and if I find an attached tick on one of them, she is willing to dose with a prophylactic dose. Testing for tick diseases is not effective until approximately 6 weeks after a bite! Too long to wait if there was exposure to disease, it’s best to treat right away.
I misunderstood about his exposure. It sounded like there were times when he had ticks on him. Yes, there are small ones and they are very hard to find, so exposure can happen without ever seeing a tick.
In general tick diseases are spreading, esp due to climate change, at a rapid rate. Areas that had no reported ticks even 5 years ago are seeing them in greater numbers, for instance Canada. I keep track of reported tick disease with this website.
http://www.petsandparasites.org/parasite-prevalence-maps/#2017/all/lyme-disease/dog/united-states/
An owner can drill down through the maps to their own county and can also request a monthly email notifying of the reported cases of each tick disease in their area. CAPC is careful to point out that these are only reported cases and the numbers of disease are probably much higher if you consider all the dogs that went untreated or vets that didn’t report. So I have been seeing skyrocketing tick disease numbers in the location I live and vacation in. You might want to keep track of CAPC maps on your own, via their regular emails.
Many owners have remembered that their pet was acting sluggishly in the days before they truly noticed something seriously wrong, you are not alone.
A PCV of 28% is great! He’s moved very close to what could be considered moderate to mild anemia. So there is positive regeneration and apparently less or no more hemolytic damage occurring.
Whatever the trigger, it appears that he was uncomfortable. Dogs tend to have behavior changes when there is some degree of pain or discomfort. So something did happen, but what is not clear.
Please keep us up-to-date with future improvements and questions!
my best patrice
Alberto,
Thank you for the complete history, this is very helpful.
This is actually babesiosis and is known in dogs while piroplasmosis is referenced in horses, not dogs. Similar diseases but babesiosis is what you are looking at now. Some breeds can actually be carriers of this disease, such as Pit Bulls, and pass it on during fighting with other dogs. It is certainly very well known in the US, with Greyhounds another breed severely impacted.
Babesiosis is a tick disease and the spleen is the organ that is most active in fighting it off. In fact, when the spleen must be removed due to illness in humans or dogs, doctors or vets will recommend that they avoid traveling to other countries where they can contract babesiosis, as the spleen has the greatest ability to control the disease. Without a spleen, it is difficult to survive this condition. Once the disease is brought under control by the body, it often remains dormant and can return in the future. Your vet used one of the most important drugs to fight it and I am so happy that they thought to use this.
So the spleen will be enlarged when there is infection by babesiosis. The spleen is a very active contributor to our immune system functions. It produces some of our white blood cells, it cleans the blood of old blood cells and it looks for and destroys RBC that contain parasites.
One of the routine functions of the spleen is to evaluate the health of RBCs. So when the body is at rest, the spleen will sequester a lot of blood. It has circuitous and convoluted pathways that require the RBC to squeeze through. Old cells fall apart and are scavenged for “parts.” RBC that contain parasites such as tick diseases will be destroyed by the immune system during this process. One sign that this is occurring is to see spherocytes in the blood. These are RBC that have had a part of them pinched off, or bitten off, by the spleen. They are smaller round, not concave, cells.
In IMHA, immune mediated hemolytic anemia and AIHA autoimmune hemolytic anemia, there is destruction of RBC in circulation. This can be assisted by the spleen. The spleen can become overactive and begin to destroy way too many RBC as well. In earlier times vets sometimes removed the spleen to stop this destruction. That surgery has mostly gone out of favor as it wasn’t shown to be completely effective in stopping the immune damage.
If you are offered to remove the spleen, I would get a second opinion. The spleen is particularly important in keeping the babesiosis under control.
A friend keeps a website about tick diseases and it would be important for you to read what she has collected.
https://sites.google.com/site/tickbornediseaseindogs/babesiosis
Now for the bone marrow. I actually have an important paper for you to read about the effects of babesiosis on dog’s bone marrow on our website. Go to this page:
https://www.secondchanceaihadogs.com/parasite-resources/
And scroll to the bottom and click on this paper:
Evaluation of blood and bone marrow in selected canine vector-borne diseases
It will open the paper in a small window, click on the arrow in the right hand corner to make it full screen. You can save and print the paper as you wish once you have done this. It is a difficult read and I don’t expect you to understand most of it, but I did want you to have something in your hand that mirrors the findings of your bone marrow biopsy.
If I could explain this the in a way you might understand, it would be to show you a picture of what the cells look like inside of the bone marrow. Each type of cell goes through a series of stages that transform it from the same basic template cell (precursor) to the mature stage. This should allow you to hover over these words and see a graphic of these cells: HSC Hematopoietic Stem Cells This is a simplified presentation of what is really a far more complex series of events. The bone marrow biopsy is looking at all these cells and evaluating the health of them and how many there are. Some are showing damage at certain steps along the way and that indicates maturation arrest. The immune system is responsible for this damage inside the bone marrow and is immune mediated bone marrow failure.
So what is the best treatment? I want you to read and print a protocol developed by Dr. Dodds of Hemopet.org. IMMUNE MEDIATED HEMATOLOGIC DISEASE and BONE MARROW FAILURE. Go to this page:
https://www.secondchanceaihadogs.com/hemopetresources/
click on the picture of the title of the protocol and it will open in the window, click on the upper right arrow to make it full screen.
This protocol is designed to hit the bone marrow with very high dose immunosuppressives. I used this protocol to save Chance’s life when he was diagnosed with a similar (but slightly different) bone marrow failure. Dr. Dodds helped me for a year while we treated him and his health was restored. The recovery happened specifically when I put him on this protocol and we introduced the high dose cyclosporine (Atopica) treatment. It took about 4 weeks at the PULSE DOSING treatment, which she outlines carefully in this protocol, make sure you vet sees this!
I also strongly suggest you contact Dr. Dodds for an owner consultation. She can further advise you on exactly how you should be dosing him with these meds and what the prognosis is that you can suppress the babesiosis sufficiently. The link to that site is on the same page, second from the top. Owner Consultation. It is $150 and she will evaluate your paperwork and advise you. She will even consult with your vet. Please let us know if you need help to do this.
Dr. Dodds saved many of the dogs that we have helped on this site. This is what she does all day long and has done for over 35 years, canine blood diseases and canine blood bank resources. She is compassionate and will be concerned about Skye.
Do you have more questions for me?
my best, patrice