Forum Replies Created
Hope,
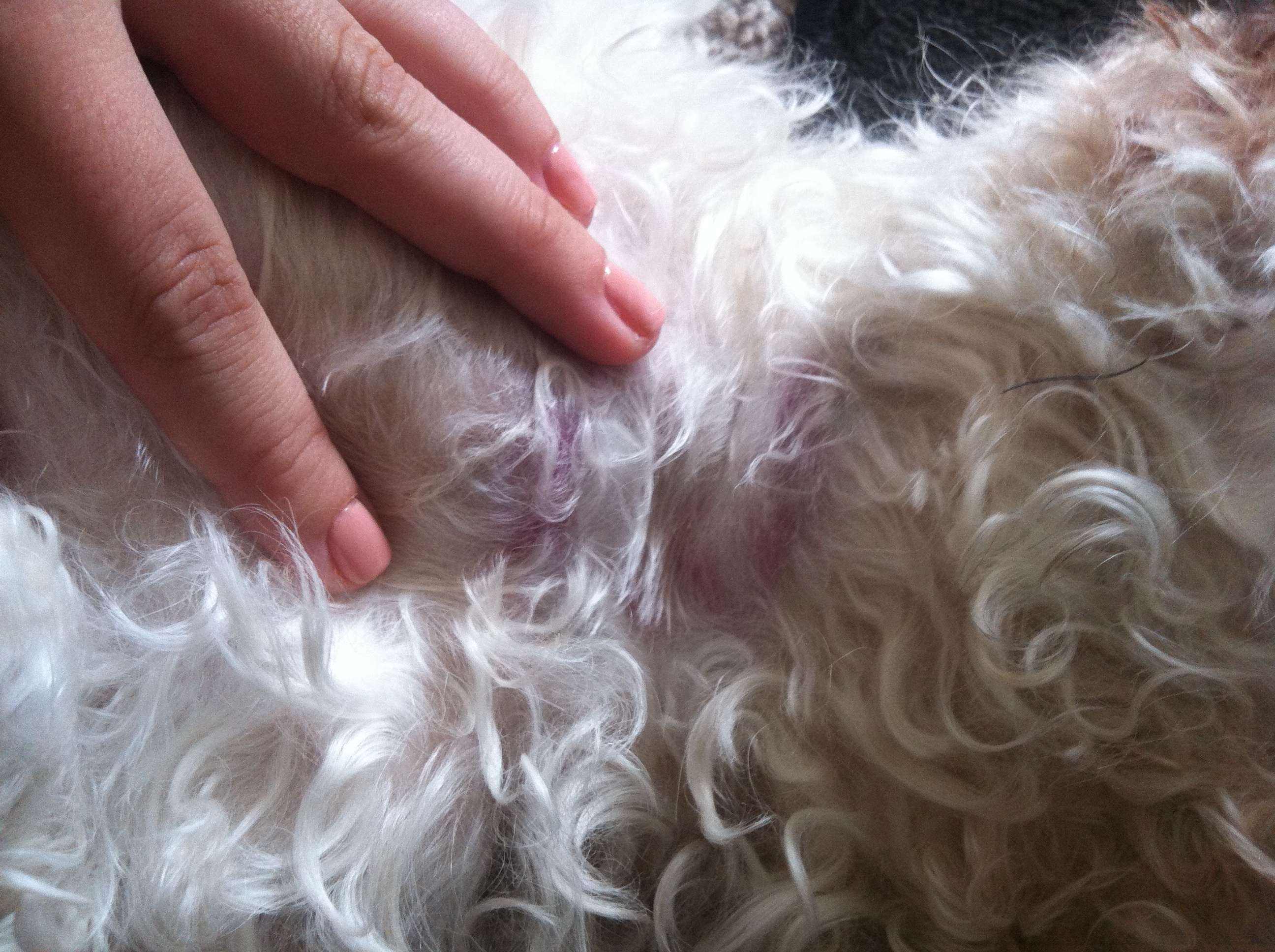
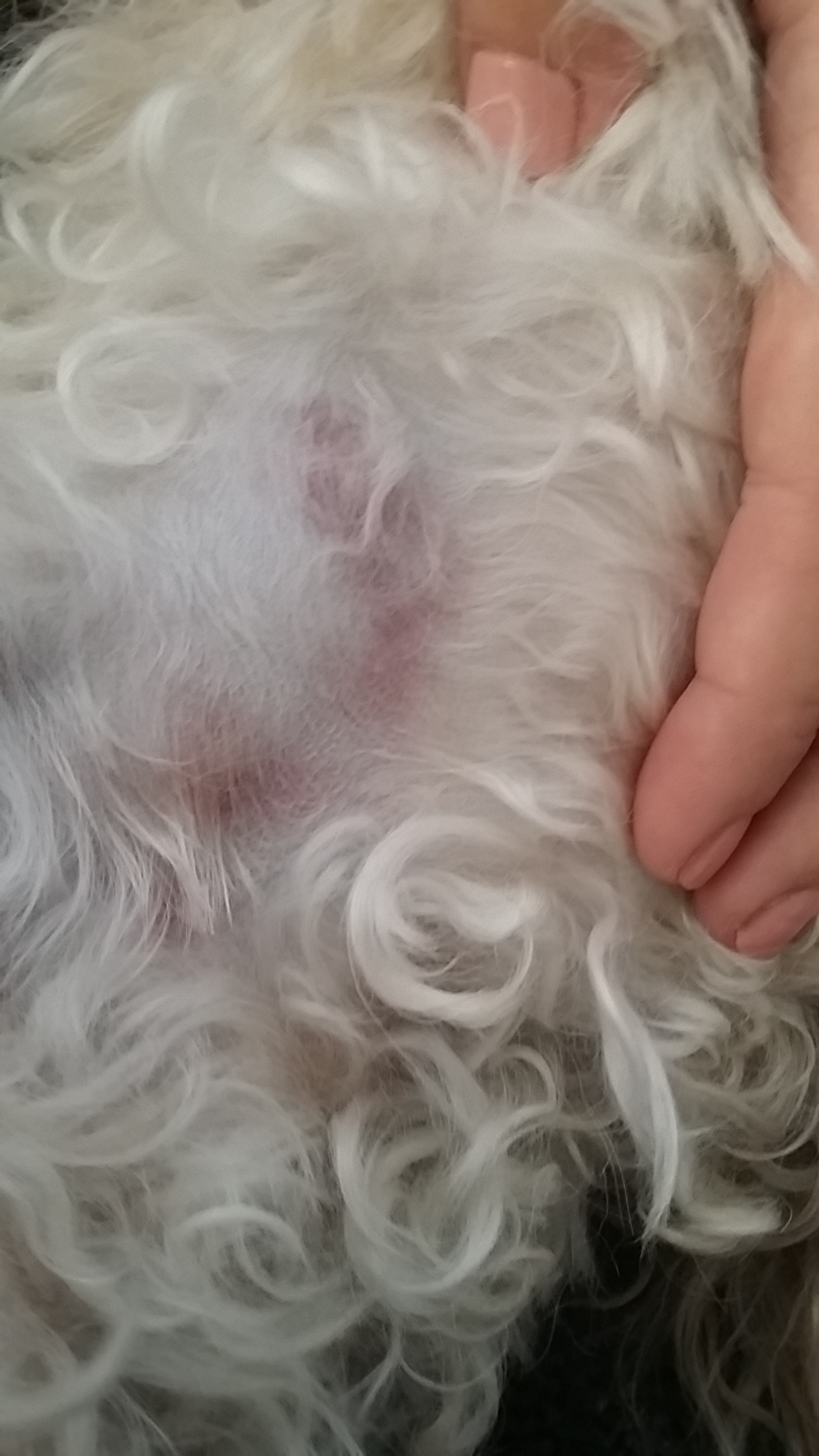
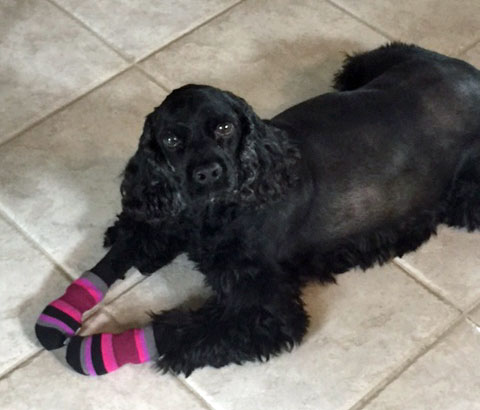
The bumps and sores are due to high dose prednisone use. Please go to this page:
https://www.secondchanceaihadogs.com/dermatology-resources
and read the two articles about Hyperadrenocorticism. Atopica (cyclosporine) can also have some skin side effects such as excess growth of the gums and a few related skin growths.
But for the most part what you are seeing is the beginnings of a staph infection which can be treated easily with an antibiotic. See this page for more information:
https://www.secondchanceaihadogs.com/AIHA_Terms/staph-infection.
Dr. Dodds has always approved Interceptor, on a 45 day cycle, for dogs on our site. I have used it for years on my dogs, safely. I like it because it also worms for more dangerous worms a dog can contract.
my best, patrice
Jen,
I’m sorry to read this. One of our past moderator’s Poodle developed this and I am wondering if she would be willing to help with the owner. Her Poodle improved but then relapsed quickly.
So that is something to keep in mind about the treatment protocol, don’t get too overeager to get off the drugs. In some of these dogs Dr. Dodds recommends a lifetime of lower dose prednisone to prevent this from happening.
I’d rather see that than for this poodle to relapse.
my best, patrice
Maria,
It’s often the case that owners are very eager to “nail” the cause of the AIHA IMHA. The reality is that in many cases they will never know what caused it. It’s good to try to associate recent events with the onset of the symptoms but sometimes it can become burdensome as the owner begins to rack their brain trying to figure out what they did wrong and what did they miss.
When Chance was seriously ill I too was trying to find the cause because even the specialist was unable to determine a cause or come up with a treatment. I have medical training and so I began to study veterinary hematology to try to find answers. That is when I began to understand his condition better. But I have to tell you that it’s been 11 years since he first became sick and I am still finding new information about what was really wrong, research that simply was not available in 2007.
So it sounds like the techs, when trying to remove the tracheal tube after the surgery, had trouble and essentially scarred the trachea and esophagus. But it wasn’t the quantity of the acid but probably rather acid reflux backing up into the esophagus that was bothersome. A dog’s stomach acid is quite acidic, usually around 1-3 pH, whereas most human’s stomach acid is 4 pH and above. This is normal in dogs and how they digest their food properly. But acid reflux is a dangerous condition because it can damage tissue and is likely contributed to his serious problems. Those delicate tissues in the throat are not meant to tolerate extremely acidic conditions.
AIHA is autoimmune hemolytic anemia. Let’s break it down: Autoimmune simply means that the immune system has become intolerant of “self.” Hemolytic means: hemo (blood or blood cell) while lytic or lysis means the destruction of the cell. So self destruction of the body’s red blood cells (in this circumstance, there are many autoimmune conditions in dogs an humans but they all area similar, intolerance of self.) This was a common term used for many years, without clear evidence of what the title really meant. But now-a-days we could say that this is an attack on “self” that seems to unprovoked, the immune system simply became intolerant.
IMHA is immune mediated hemolytic anemia. So broken down. Immune obviously involves the body’s immunity against disease, invaders, parasites etc. Mediated mean helped by, assisted by or brought about by, so the condition is mediated by some force, whether it is identifiable or not.
But in more recent years researchers and vets are becoming more convinced that most of the cases in the past they felt were just the immune system going haywire on its own were really caused by some trigger or triggers.
So now the diagnostic science of these conditions is slowly turning in the direction of attempting to identify the outside factors, the triggers and the direct causes of the immune system becoming intolerant of “self.” Thus, initial visits are becoming more lengthy, with more diagnostics and more opportunities to save dog’s lives. So IMHA is really the more correct terminology, “something” mediated the immune system to begin attacking its own red blood cells. It honors the science of diagnostics as a valid approach to treating canines.
This is really why I made this website, because I believe good diagnostics are the keystone to saving dog’s lives. If your car seems to be driving funny, you might sit in the driver’s seat for an hour worrying about all kind of things like maybe you will need to have the engine rebuilt. However it you get out of your car and actually look at your car you might see a flat tire.
A third companion to AIHA and IMHA is some form of bone marrow failure, a far more serious and difficult condition to understand and treat. This is what Chance had an he was literally not making RBC or white blood cells (neutropenia.) A true death sentence if we couldn’t figure out how to help him make blood again.
So it appears the vet did several of the gold star diagnostics which is super. That goes a long way in demonstrating that they were trying to find every possible treatable trigger they could. I don’t think you need to quiz your vet on the things I have mentioned. They were questions I had about his diagnostics that have been answered.
Ok, so you did decrease the prednisone by 25%, excellent. That is exactly what we recommend here on Second Chance. Read the page link I posted yesterday about how to proceed with further reductions. This is as much as you should decrease in about every 3-4 weeks.
Questions are good, they help you learn. So you asked about how infections or other invaders of the body that alert the immune system can lead to AIHA IMHA. Good question.
There is a condition we see regularly here on Second Chance that leads many dogs to continue to have a chronic or refractory anemia. This means it is difficult to treat. This is often related to “anemia of chronic disease.” The body, when trying to fight invaders, attempts to withdraw resources from the invader so they have less of the materials they need to survive.
So let’s say we have an infection that has led to an inflammatory condition. There is a release of inflammatory cytokines like tumor necrosis factor and the interleukins etc. into the body. This suppresses the production of red blood cells in the bone marrow. In addition the body begins to attempt to reduce the amount of iron available to the “invader” and withholds it from circulating in the body. Thus the bone marrow doesn’t get enough iron to properly produce new red blood cells. The are poorly made and ineffective, leading to a chronic low grade anemia. In these cases the original condition cause must be discovered and treated before the dog will begin to recover from anemia. How all this works is simply amazing. The body is simply restricting its resources to make blood while it attempts to destroy and drive out invaders such as infections.
Since he has had serious gastrointestinal problems in the past it would be worthwhile to have him tested for several important nutrients, folate, cobalamin (B12) and possibly iron. See this website for an extensive explanation for why there can be cobalamin deficiencies in gastrointestinal diseases. My Chance had a deficiency of B12 due to malabsorption and I supplemented him at home with B12 shots.
http://vetmed.tamu.edu/gilab/research/cobalamin-information
These nutrients are critical for the making of blood, without them there can be a continued manufacture of poorly made RBC which have trouble surviving and tend to have a lower hemoglobin count. The tests can be done via this lab.
My best patrice
Hi Maria,
I have your tests in front of me, thank you for sending them! They are from earlier this year, do you have anything more recent?
On the summary from 6-20-18 the report indicated that ” Labwork showed mild regenerative anemia.” But then the report goes on to state that there is value of 379,200 reticulocytes. These two things do not match (mild regenerative anemia and this extraordinarily high retic value.)
Here are the reference values from Cornell to match the number of reticulocytes to the degree of regeneration.
Degree of Regeneration Absolute reticulocytes (/uL)
None < 95,000*
Mild 100,000
Moderate 300,000
Marked ≥ 500,000
In addition, anemia is defined as none, mild, moderate or severe. On this test the HCT was 39% which can be considered none to mild depending on the lab references.
Reticulocytosis is an increase in the production of immature red blood cells in the bone marrow in a response to anemia. The lower the HCT, the greater the number of reticulocytes must be produced to normalize the blood. In this case, since Hunter was at 39% HCT, his body should have been only making about 60,000-80,000 reticulocytes not 379,200! Why is this?
The comments under Erythrocytes (which are red blood cells) is wordy but it is simply identifying that there are differences in the size and coloring of the RBC. For instance reticulocytes are larger for about 4-5 days than RBC and they have a “reticular” patterning inside which makes them a different color. (“marked
polychromasia with increased numbers of nucleated red blood cells.”) They quickly drop the reticular (nucleated )pattern which is really the RNA inside the cell and begin to look more like a RBC.
So to be clear the whole process of rapidly making reticulocytes in great numbers and sending them out into the blood earlier than normal leads to a lot of differences in cell types, sizes and coloring which is exactly what all the words on the lab report are saying.
So later in the report in the Interpretation they note “Markedly regenerative anemia.” I can’t be sure why they said it wasn’t and then it was from the same report.
What is important is that there were a large number, 50%, of spherocytes. These are RBC that have a little “bite” taken out of them. They appear smaller, less concave, and paler than normal. In many cases with this many circulating spherocytes it is an indication that the spleen has been very busy attempting to destroy RBC by taking a “bite” out of them, in an attempt to remove them from circulation.
The most usual case is that the immune system is targeting these RBC for destruction and that is the job of the spleen every day, to get rid of old worn out RBC, but certainly not in large numbers. But if the cells contain something like a tick disease and that could trigger this destruction. But the immune system can also become errant and begin destroying these marked RBC for the wrong reasons.
The lab also notes “Spherocytes can also be seen with blood transfusions and zinc
toxicity. ” So the question is did they do any transfusions and did they investigate the possibility that Hunter may have swallowed a coin? Some older coins contain zinc. Or it could be possible that something you gave him contained zinc.
I am very leery of rawhides. They tend to be swallowed in chunks that are glue-like globs and they compact in the intestines causing digestive blockages. Throw any you might have left away, please.
Now I am looking at the April 21 report, first the chem screen.
The first thing that is abnormal is the high-ish Globulin level (3.8, normal high is 3.6). There can be a variety of reasons why this is a bit high. Ehrlichia (tick disease) or heartworm infection, chronic liver disease, auto-immune diseases, chronic infections, inflammatory responses and dental disease. Most of these things can be tested for and treated.
ALKP is a bit high at 161 (high normal 131) but that it isn’t very high. This is an enzyme released usually by the liver when there is cell damage. It is quite common when prednisone is being taken as the liver processes this drug and we always expect to see this value rise while on prednisone. Once it is removed the value will go back to normal.
Bilirubin is just a touch high and that is usually a sign of RBC destruction. So we must be looking at the tail end of whatever occurred in the recent past before these tests. All other chem screen value are normal. This is a sign of a relatively healthy dog.
On the CBC it is important to note this comment: “Agglutination observed; hemogram may be affected” This means that there was some damage to the red blood cells during handling, either during the blood draw or afterwords the tube was mishandled. This changes many of the values on the test and skews the results. It is important that the tech get this job done correctly.
MCV mean corpuscle volume is a touch high, 80 vs normal 79. It simply is noticing the number of larger reticulocytes.
NRBC nucleated red blood cells, again this is the reticulocytes with their RNA still inside, this is considered a sign of retitculocytosis, or the making of many new red blood cells. It should be high considering there are 379,200 reticulocytes!
Monocytes are 1% higher than normal, and the absolute value is 902 vs high normal of 840. These are the vacuum cleaners for the bad stuff in the body, which is usually an indication of infection.
Again, let me mention again, the Reticulocyte percentage is 7.9 with an absolute value of 379,200. I usually only see values like this in dogs with a HCT of 9-12%, not 39%!
So it is possible this was AIHA IMHA. If so we are looking at the tail end of the event, as he appears recovered. I am not sure why your vet is not satisfied with these values. I should also note that in some cases there is a small internal bleed that can lead to this kind of high retic values and that could be a small tumor or perhaps a stomach ulcer due to the prednisone or a bout of serious bowel inflammation (colitis.) Have these things been checked for? Did the vet tell you to use some kind of stomach protection to protect against ulcers? If not use the generic version of pepcid, on regular tab 30 min before the first meal of the day. One per day is enough.
In any case, if you are using cyclosporine it is possible to begin decreasing the prednisone carefully as the cyclo is doing the main job of immunosuppression. If you are seeing rear leg weakness and trembling then it indicates that he needs to have this dose reduced.
Here are my recommendations for reducing prednisone. Do not do this without your vet go ahead! This must be done very carefully and you need your vet to monitor Hunter during the process.
https://www.secondchanceaihadogs.com/AIHA_Terms/prednisone-dose-reduction
What questions do you have for me?
My best patrice
Angela,
Welcome to Second Chance. I am sorry to read about Maude. This is indeed a very sudden event.
A severe reaction like this to a sting or bite is unfortunately common enough to be part of the known triggers for autoimmune hemolytic anemia in dogs. In this case we could call it IMHA or immune mediated hemolytic anemia because we know that this was “mediated” by a known trigger. These triggers can be numerous and variable. Many breeds have a genetic predisposition to autoimmune diseases and the immune system will react when enough of the triggers are present. So it is often a whole group of triggers, not just one, that leads to IMHA. It’s quite possible that once she was stung her immune system became alert to many other things like medications etc. For example we might see an older female, perhaps a breed like a Cocker Spaniel, in heat (lots of hormones), who may be overweight (inflammatory influences) and the vet suggests that she”get that yearly booster shot to protect her.” This can and often leads to the expression of IMHA.
The term AIHA is considered being more of a primary cause for autoimmune hemolytic anemia. The immune system is triggered by an unknown trigger. And there are plenty of times where owners and vets never really can pinpoint exactly what triggered the condition.
Luckily, the acute care is usually the same, high dose immunosuppressive drugs such as prednisone. This suppresses the over activity of the immune system in an attempt to stop it from attacking and destroying red blood cells. But you are probably guessing that longer term use of this drug has some serious side effects. What is long term? We should hope for almost immediate responses but some dogs need longer periods of time to stop hemolysis. They may need one or more transfusions to give the drugs time to work.
What is critical during this period of time is for the vet to begin looking for other triggers that may be contributing to the condition. If there are other treatable causes then it will be very helpful to start treatments. For instance tick diseases are a frequent trigger and treating the dog with doxycycline immediately kills the tick disease and the immune system reduces the attack. In young dogs they often put everything in their mouths so we look for ingested coins or older style rat poisons. Older dogs can have tumors that can be a trigger. Vaccines are part of these triggers. Dogs that have had previous autoimmune conditions such as developing atopic dermatitis (canine inhaled allergies) at a young age will be prone to developing AIHA IMHA. Digestive disorders seem to be very complicit in the development of autoimmune conditions. The inflammatory conditions that develop in the intestine contribute. The pancreas, as you mentioned, can also contribute indirectly and we might see this as more of a non-regenerative anemia due to poor nutrition absorption.
Severe acute cases can be a difficult balancing act because the homeostasis of the circulatory system becomes compromised. Red blood cells being destroyed in circulation create a large load of intravascular debris and organs such as the liver and kidneys have a hard time processing it. You may see jaundice for instance as unprocessed waste builds up in the blood. Since you are a nutritionist, you will understand that we want to reduce the wastes that these organs are trying to process by, for instance, avoiding red meats in the diet that add even more red blood cell wastes. The liver is already being compromised by processing the prednisone (you will see the liver enzymes rise during treatment) and so we often recommend the liver sparing diet. See this page for the diet, click on the picture for Liver Sparing Diet and it will open a window, you can then click on the upper right hand arrow to open it in a full tab where you can save or print it.
https://www.secondchanceaihadogs.com/nutrition-resources
Another unfortunate condition of acute hemolysis is a breakdown of the normal clotting process in the blood (called the clotting cascade.) We often have small injuries in the blood vessels and the body is very good at quickly clotting these. But with the instability of hemolysis comes a greater risk of inappropriate clotting. The medical term for this is DIC disseminated intravascular coagulation. The body begins to sense that there seems to be injuries everywhere in the blood vessels and it begins to try to fix everything all at once. Fibrin strands begin to form in many places and clots develop. Thus we almost always recommend an immediate discussion with the vet about the use of low dose aspirin or other clinical drugs like heparin (dosed carefully for dogs.) In the early acute days clotting can be a difficult condition to manage.
Transfusions are helpful and you may experience a rise in the PCV HCT but then the next day see it fall. This is expected. But the important things about the transfusion are the additional elements of the blood such as serum, this helps reduce hypovolemia, which is low fluid volume. Transfusions improve homeostasis. Each transfusion after the first must be matched and typed. Transfusions must be done slowly to avoid transfusion reactions! After a few weeks, transfusion triggers should be carefully evaluated by an expert to determine if the need for another one is called for.
So in general you are asking “what should I be doing?” First, remember that you want to be included as part of the team that helps Maude. Be polite and calm at all times. Request nicely but firmly that you want to be included in all clinic activities with her, excluding of course xrays. You want copies of all her lab and blood work (which you can upload to me on the Urgent Advice page.) Your vets know you are upset and worried, so your job is to be focused on helping get Maude better, not expressing your out of control feelings. Maude will sense your panic and fear and then feel she has done something wrong. Be cheerful and happy around her.
Read everything you can on this website. We have put up a ton of information for you to study. Ask me questions about anything you aren’t sure about. Read Our Stories to get a feel for how this condition can be so variable from one dog to the next.
Most of all, we want you to make decisions based on your knowledge, not on your emotional feelings. Since you are limited in time, you can’t possibly understand everything you need to do that right now! Trust us to guide you with the decision making processes. Vally and I both had dogs that were seriously ill and we understand how you feel right now. Panic and fear.
Vally will hopefully pop in later and advise you about some supplements that should be added to Maude’s protocol. She can even make up a chart to help you dose everything properly!
What questions do you have for me?
my best, patrice
Admin note:
“ATOPICA should be stored and dispensed in the original unit-dose container at controlled room temperature between 59 and 77°F (15-25°C).”
See:
https://docs.google.com/viewerng/viewer?url=https://www.secondchanceaihadogs.com/wp-content/uploads/2015/04/atopica-product-insert.pdf
I asked Dr. Dodds who advised that I should check with the manufacturer who responded with the same information: stored between 59 and 77°F .
If dosing it is causing diarrhea, vomiting and other stomach upset then it can be given with food for a few days. Most dogs in the study (read the product insert) adjust to it after a short period of time.
I suspect freezing damages the preparation of the “microemulsion in an aqueous environment.” Specifically it is a cyclic polypeptide “metabolite by the fungal species Beauveria nivea” consisting of 11 amino acids.
PJ,
Good to see you back!
First, Stella no longer is considered anemic. Her HCT hematocrit, 42.2% is well within normal limits (wnl.) The reference range is 37.3-61.7.
Since there is no anemia at this point, the body has basically slowed down the regenerative process in the bone marrow to a normal level of about 1% and 50,700 absolute reticulocytes. All humans and dogs have this normal level of reticulocytes. There is no reason to continue to suppress the immune system with the higher doses of immunosuppressive drugs (prednisone, azathioprine, or cyclosporine). If you are still using high dose prednisone it is ok to start reducing that very slowly. See this page:
https://www.secondchanceaihadogs.com/AIHA_Terms/prednisone-dose-reduction
There is one value that relates to the red blood cells that is somewhat high, called MCV mean corpuscle volume, the size of the RBC, and this case the cells are larger than normal. Because of these larger cells, this has caused the HGB hemoglobin amount to look a bit low, 12.6. HGB reference range 13.1-20.5.
The HCT hematocrit is fine and the lower hemoglobin is negligible. Sometimes when a dog has had AIHA IMHA, replacement RBC’s made in a hurry are a bit too large when they are new and I suspect that another CBC in the future will not look the same.
However, the WBC white blood cells count is a bit high, 19.29. The reference range is 5.05-16.76. This is a combined count of all 5 types of WBC and these are your defensive cells of the immune system. Each type has a different job.
Neutrophils NEU are in the greatest quantity in the body and when they become high we usually suspect infection of some kind. On this test, NEU is 16.10 with a reference range of 2.95-11.64.
Monocytes MONO are called macrophages, WBC that vacuum up unwelcome things in the body. They become very active when other WBC attack bacteria etc, cleaning up the “mess.” The value on your test 1.21 is slightly high, reference range 0.16-1.12. Not a really high value, but indicative of some kind of inflammation or infection that has occurred.
Finally the basophils BASO are high 0.42, reference range 0.00-0.10. It is rare to see basophils at all and any amount above normal should be noted. Their job is usually related to allergies and if you see higher eosinophils EOS also, this is a good indicator that a dog may have an allergic reaction. However in this case the EOS values are normal. So a vet might think along the lines of something amiss with the bone marrow. I would want to see previous CBC’s to see what has been happening up to this point. One test doesn’t tell a very good story, multiple tests show changes and trends.
On the chem screen there are number of values that are high.
BUN blood urea nitrogen is a kidney function value and this indicates the amount of wastes that the kidneys were not able to process properly that remain the blood. In this case the value is 28 reference range 7-27. So it’s not very high. In a case like this we would also look at another value called creatinine to see if it is high also, in this case it is normal. So then we would look at their ratio. In this case the ratio might appear to be normal. Since the kidneys are so critical and BUN can indicated damage it would be important to check with the vet to see how they feel about this slightly high value. Viewing multiple chem screens might show a trend.
ALT Alanine transaminase and ALKP Alkaline phosphatase are liver enzymes that usually indicated that liver cells are being damaged. The ALT is high, 534, reference range 10-125. ALKP is high 296, reference range 23-212. When your dog is on prednisone, the liver processes this drug and during this liver cells will die. So it is pretty clear that these levels are high because of the use of high dose prednisone. This is a very normal and usual consequence of treating any dog with AIHA IMHA. There should be no cause for alarm, if there was no organic liver disease prior to now, once the prednisone dose is reduced these values will return to normal. But we can help the liver with a supplement. In this case they used what I always recommend, Denamarin. This is a high quality liver supplement dosed appropriately for dogs. You should continue this supplement for the whole period of time you are also giving prednisone. While these values appear high, many dogs will have extraordinarily higher values when on prednisone and they do recover as the liver is regenerative.
GGT Gamma-glutamyltransferase is also an indicator, usually, of liver problems. It is high, 58 reference range 0-11. In this case I think the vet would agree this is another indicator that the prednisone is the source of the liver injury and once reduced this value will decrease.
Finally the CHOL cholesterol value is high 386 reference range 110-320. Dogs do NOT have the same kind of cholesterol problems that humans do, it is a very different species when it comes to blood levels of CHOL! Dogs are capable of handling fats very differently than humans and they are every efficient at converting fat to blood glucose, their main source of energy fuel. They can survive quite well without added carbohydrates to their diet, producing their blood sugars with converted fat. So why is the high CHOL value of concern? Well the first reason is simply that the dog was not fasted properly before the blood was drawn, there should be a fast of at least 8-10 hours before this, and there is a lot of fat remaining in the blood, called lipids, which can interfere with many values on a blood test. If we could look at other previous tests and see the CHOL is consistently high then I would suggest that there may be hypothyroidism and would recommend a full thyroid panel be done, Hemopet can do this. In dogs, the CHOL is a very accurate indicator that the dog has hypothyroidism, nearly 75% of dogs that are hypothyroid will have elevated CHOL. See this page and select the Thyroid Profile 4 (T4, free T4, T3, free T3). When you select this test, it will give you instructions how to draw and mail the serum sample to Hempet.
https://labordatenbank.com/cake/hemopet/samples/hemopet_form
So first, please get me some early test results. I would recommend a slow reduction of prednisone and if the cyclosporine is dosed higher than a regular maintenance dose then reduce it to a maintenance dose for now and then once the prednisone is reduced you can begin to reduce the cyclo at a slow rate. It is more important to reduce the pred now so as to reduce the load on the liver.
Do not add any supplements like this to the regimen. If anything the diet and supplements should be carefully monitored to optimize liver support and anything new should not be added since we do not know how it could affect the liver. I suggest that you use Dr. Dodds Liver Sparing Diet. see
https://www.secondchanceaihadogs.com/wp-content/uploads/2015/08/Cleansing-Diets.pdf
my best, patrice
Taylor,
Oh I am so sorry. I was really hoping he would pull through this. He was in the right place and I believe the vets did everything in their power to help him.
I have been thinking about this for days and I believe that he must have contracted a tick disease a long time ago, as you said he was covered with ticks, and was either treated or his immune system fought it off at that time, but not without some damage. His kidneys could have been partially affected, as we know dogs can survive quite well with reduced kidney function. You may have never noticed it and could not have anticipated this happening. The efforts you went to helping him are a testament to the great love you have for him.
Harley had a wonderful life with you and your care has kept him healthy and happy for many years. Please know that he loved you very much and his joy was that you were with him. He would not want, in his doggie way, for you to feel guilt or sadness. That is our hardest job as owners, not feel tremendous guilt. The rough edges of your grief will soften over time and you will remember the good times and these bad spots will fade into the back of your mind.
Please come to us when you need to talk, we are always here and welcome you at any time. We all understand here.
My deepest condolences to you for your great loss
Love, Patrice